Urticaria, often known as hives, is a skin disorder that causes swollen, itchy, and frequently red welts on the skin. Hives can form anywhere on the body, vary in size and shape, and are frequently present in clusters. If you have urticaria symptoms, it is critical that you seek medical assistance to discover the cause and obtain appropriate treatment. Most cases of urticaria can be adequately treated and controlled with the proper therapy.
Understanding Urticaria and Its Symptoms
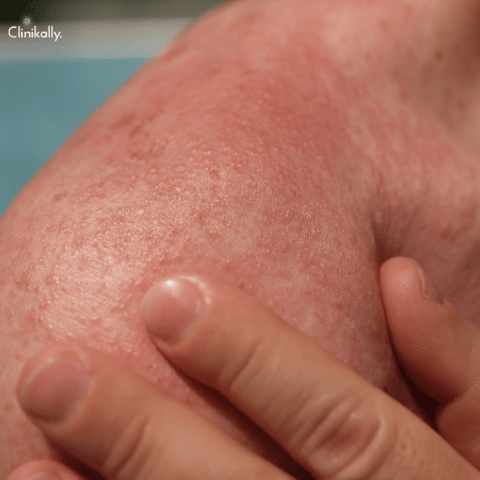
Urticaria, also known as hives, is a skin disorder characterized by the formation of red, itchy, and swollen lumps on the skin. These lumps can vary in size and shape and can appear anywhere on the body. Depending on how long it lasts, urticaria can be acute or chronic. Acute urticaria, which typically results from an allergic reaction to food, medication, or insect stings, lasts less than six weeks. The cause of chronic urticaria, which lasts longer than six weeks, may be an autoimmune disease, a thyroid condition, or another medical condition.
Urticaria signs and symptoms include:
-
Bumpy skin that is red or pink in color
-
Itching
-
Swelling
-
Stinging or burning to feel
-
Blistering
-
The appearance of redness around the eyes, lips, or tongue (angioedema).
Other symptoms such as fever, fatigue, joint pain, or difficulty breathing may accompany urticaria in some cases, indicating a more severe allergic reaction.
Acute vs. Chronic Urticaria
Urticaria is characterized as acute or chronic based on how long the symptoms last. Hives that last less than six weeks are referred to as "acute urticaria." There are numerous potential causes, such as:
-
(Viral or bacterial) infections
-
Antibiotics and nonsteroidal anti-inflammatory drugs are examples of medications.
-
Insect stings or bites
-
Allergies to certain foods (such as nuts, shellfish, eggs, or milk)
-
Pressure, cold, or heat are examples of physical stimuli.
-
Stress
In contrast, chronic urticaria is described as hives that linger for more than six weeks. Chronic urticaria can be difficult to diagnose, but it may be associated with an underlying autoimmune illness. Other potential causes of persistent urticaria include:
-
Physical cues (like pressure, cold, or heat)
-
Infections (including hepatitis and HIV)
-
Thyroid problems
-
Chronic idiopathic urticaria (cause unknown)
Chronic urticaria, which can be persistent and difficult to manage, can have a significant impact on a person's quality of life.
Common Triggers and Allergens
The following are some of the most common allergens and triggers:
-
Food allergies: Typical food allergens include shellfish, milk, eggs, and peanuts.
-
Medication: A number of drugs, including aspirin, nonsteroidal anti-inflammatory drugs (NSAIDs), and antibiotics, can cause hives.
-
Insect bites or stings: Mosquitoes, bees, and other insects can cause hives in some people.
-
Latex: Latex-allergic people may experience hives when using latex products such as gloves and condoms.
-
Heat and cold: For some people, extreme temperatures can cause hives.
-
Stress: For some people, emotional stress can cause hives.
-
Exercise: A type of hive called exercise-induced urticaria appears during or after physical activity.
-
Infections: Hives may occasionally result from bacterial or viral infections.
It is significant to note that hives frequently have no known cause. This is known as idiopathic urticaria.
Diagnosis and Treatment Options
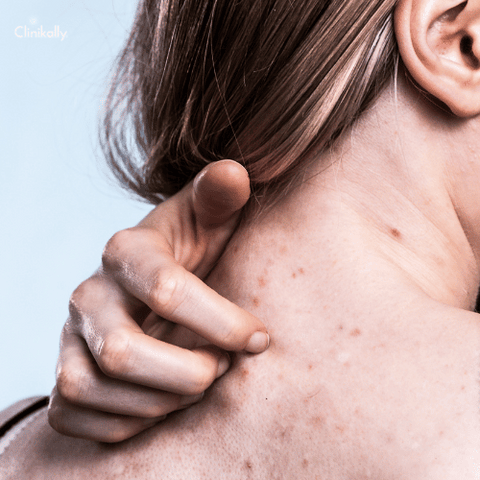
A physical examination and a review of medical history are used to identify triggers and probable underlying causes of urticaria. To discover the cause of the hives, allergy testing or blood tests may be recommended in some circumstances. Urticaria is often treated by recognizing and avoiding triggers, as well as taking antihistamines to relieve symptoms. Over-the-counter antihistamines such as diphenhydramine or loratadine may be adequate to relieve the symptoms of acute urticaria. Higher doses of antihistamines or other drugs, such as omalizumab, cyclosporine, or corticosteroids, may be recommended for chronic urticaria.
Other measures to relieve symptoms and prevent flare-ups, in addition to medication, include:
-
Avoiding triggers: Make a list of all potential triggers and allergens, and stay away from them.
-
Cool compresses: Cool compresses can be used to soothe the skin and stop itching, as can cool baths.
-
Loose clothing: Wear loose, breathable clothing to prevent further irritation of the skin.
-
Stress management: Because stress can aggravate hives, stress management techniques or therapy may help reduce symptoms.
If your urticaria symptoms are severe or persistent, you should see a doctor for a proper diagnosis and course of treatment. Rarely, hives may be a symptom of a more serious underlying condition that needs additional testing and care.
Dermatological Evaluation
A dermatological evaluation involves a thorough examination of the skin, hair, and nails. A dermatologist, a medical specialist who specializes in detecting and treating skin disorders, is usually the one who does it. A physical examination of the skin, a review of the patient's medical history, and a discussion of any symptoms or concerns the patient may have are all part of the evaluation.
The dermatologist will inspect the skin for any anomalies, such as rashes, growths, or discoloration, during the physical examination. They may also employ dermatoscopy, a unique piece of equipment that magnifies the surface of the skin, to better see any anomalies. In addition, the dermatologist may inspect the hair and nails for signs of infection or other problems. Following the physical examination, the dermatologist will usually ask the patient about their medical history, including any prior skin diseases or treatments. They may also inquire about any current medications the patient is on, as some medications might trigger skin problems.
The dermatologist may propose additional tests or procedures to help diagnose the problem based on the examination and medical history. Blood tests, skin biopsies, and allergy testing may be included. Following a diagnosis, the dermatologist will collaborate with the patient to design a treatment plan. Depending on the illness being treated, this may include topical or oral drugs, lifestyle changes, or other therapy. The dermatologist will also usually advise you on how to avoid future skin problems and how to properly care for your skin, hair, and nails.
Antihistamines and Allergen Avoidance
Antihistamines are the primary treatment for urticaria because they prevent the release of histamine and other substances that cause hives. Antihistamines are available in both prescription and non-prescription forms. and over-the-counter versions, with loratadine, cetirizine, and fexofenadine being common examples. A doctor may prescribe a stronger antihistamine or a combination of antihistamines in cases of severe or persistent urticaria. Avoiding allergens and triggers is also an important element of urticaria management. Certain meals, drugs, insect bites or stings, and exposure to heat or cold are all common causes. Identifying and avoiding certain triggers can lower the frequency and severity of hives in some individuals.
Topical or oral corticosteroids, which help reduce inflammation and itching, may also be used to treat urticaria. Omalizumab, an injectable medicine that targets an antibody involved in allergic reactions, may also be used in cases of chronic urticaria. It may also be necessary to treat the underlying illness in rare instances where hives are brought on by a medical condition, such as an autoimmune disorder, in order to control urticaria.
Managing Urticaria Effectively
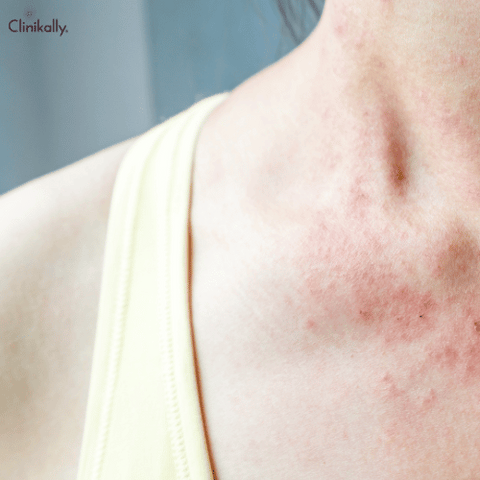
To effectively manage urticaria, identify and avoid triggers, take recommended medication, and make lifestyle changes to lower the risk of hives.
-
Identify and avoid triggers: Keeping a diary of your activities, food intake, and other factors that coincide with the onset of hives can help you identify potential triggers. Once you've identified your triggers, try to avoid them as much as possible.
-
Take prescribed medication: Antihistamines are commonly used to treat urticaria symptoms. Corticosteroids or immunosuppressants may be prescribed in severe cases. Always take your medication as directed, and consult your doctor if you experience any side effects.
-
Change your way of life: Reduce your stress levels, avoid tight-fitting clothing, and stay away from extreme temperatures, which can cause hives. You could also try relaxation techniques like deep breathing, meditation, or yoga.
-
Seek emergency treatment if necessary: If you have difficulty breathing, swelling of the tongue or throat, or feel faint, seek immediate medical attention. These symptoms could be anaphylaxis, a severe allergic reaction that necessitates immediate medical attention.
-
Follow up with your doctor: Schedule regular visits with your doctor to go over your progress and, if necessary, modify your treatment plan.
You can successfully manage your urticaria and enhance your quality of life by following these steps.
Skin Care and Inflammation Reduction
Skincare and inflammation reduction are critical components in the treatment of urticaria. Here are some suggestions:
-
Moisturize your skin on a regular basis: Dry skin can exacerbate the symptoms of urticaria. After bathing, moisturize gently with a fragrance-free product to help retain moisture.
-
Avoid hot water: Hot water can dry out your skin and exacerbate urticaria symptoms. alternatively, use warm water.
-
Choose gentle skin care products: Stay away from harsh soaps and detergents that can irritate your skin and opt for hypoallergenic, fragrance-free options.
-
Wear loose, breathable clothing: Tight clothing can irritate your skin and aggravate urticaria symptoms. Wear loose-fitting clothing made of breathable fabrics such as cotton.
-
Cool your skin: Apply cool compresses to your skin to help reduce inflammation and itching. You can also take a refreshing bath or shower.
-
Use topical treatments: Over-the-counter hydrocortisone cream, for example, can help reduce inflammation and itching. They should, however, only be used under the supervision of a healthcare provider.
-
Maintain a healthy diet: According to some research, consuming a diet high in fruits, vegetables, and omega-3 fatty acids may help to reduce inflammation in the body.
It's important to remember that while these suggestions can help manage urticaria symptoms, they might not be sufficient to address the condition's underlying cause. Consult a healthcare provider for further evaluation and treatment if you have chronic urticaria or severe symptoms.
Coping with Itchiness and Discomfort
Urticaria can cause itching and discomfort, which can be upsetting for those who suffer from it. Here are some suggestions for dealing with these symptoms:
-
Apply cool compresses: To soothe the skin and reduce itching, apply a cool, damp cloth or an ice pack wrapped in a towel to the affected area.
-
Avoid hot showers or baths: Hot water can worsen itchiness and dry out the skin. Instead, use warm water.
-
Wear loose-fitting clothing: Tight clothing can irritate the skin and aggravate itching. Choose clothes that are loose-fitting and made of breathable materials.
-
Avoid scratching: Scratching can aggravate the itchiness and cause skin damage and infection. Instead, use a soothing lotion or gently rub the affected area.
-
Moisturize the skin: To relieve dry, itchy skin, use a fragrance-free moisturizer. Apply it several times per day, preferably after bathing or showering.
-
Take an oatmeal bath: Oatmeal has anti-inflammatory properties that can help soothe itchy skin. Soak in a bath of colloidal oatmeal for 15-20 minutes.
-
Antihistamines should be taken as directed: Antihistamines can help reduce the itching and swelling caused by urticaria. However, make sure to follow the instructions on the package or as directed by your healthcare provider.
If your symptoms persist or worsen despite these precautions, you should seek medical attention.
When to Consult a Medical Professional
If the hives do not go away after a few days or are causing discomfort, such as severe itching, swelling, or difficulty breathing, it is best to see a doctor. If you have hives and additional symptoms like fever, joint pain, or a sore throat, you should see a doctor. In some situations, hives can be a sign of a more serious underlying problem that requires medical attention, such as an autoimmune disorder or an allergic reaction. A dermatologist or allergist can help determine the cause of the hives and develop a treatment plan.
Persistent Symptoms or Unclear Diagnosis
If you are experiencing persistent symptoms of urticaria or if you are unsure about the diagnosis, it is important to consult a medical professional. A dermatologist or allergist can help diagnose the condition and recommend appropriate treatment options based on your specific situation. In some cases, additional testing or evaluation may be necessary to identify the underlying cause of the hives. Additionally, if you experience severe or life-threatening symptoms, such as difficulty breathing or swelling of the face or throat, seek emergency medical attention immediately.
Seeking Proper Treatment and Advice
If you are having urticaria symptoms or suspect that you may have this illness, it is critical that you obtain adequate medical treatment and assistance. Your doctor or dermatologist can do a complete examination, provide an accurate diagnosis, and suggest appropriate treatment options. If you are already being treated for urticaria but your symptoms persist or worsen, you should see your doctor to discuss other treatment options or rule out any other underlying diseases. In addition to medical treatment, you can improve your general skin health by making lifestyle changes such as eating a nutritious diet, avoiding triggers that produce or worsen hives, and using mild skin care products.
Living with Urticaria

Living with urticaria can be difficult, but there are ways to manage the condition and improve your quality of life. Here are some pointers that might be useful:
-
Identify and avoid triggers: Be aware of what causes your hives and try to avoid them as much as possible. Certain foods, medications, insect bites, and exposure to heat or cold are all common triggers.
-
Maintain a healthy lifestyle: Eating a healthy diet, getting regular exercise, and managing stress can help your immune system function properly, reducing the frequency and severity of urticaria.
-
Management of symptoms: As directed by your doctor, take antihistamines or other medications to reduce itching and stop the development of new hives. Using cool compresses or taking a cool bath are additional ways to relieve symptoms.
-
Seek help: Living with a chronic condition such as urticaria can be emotionally draining. A support group, your family, or your friends may be able to offer you some assistance.
-
Communicate with your healthcare provider: It is critical to discuss your symptoms and treatment options with your healthcare provider. If necessary, your provider may be able to modify your treatment plan or refer you to a specialist.
Remember that most people with urticaria can live normal, healthy lives with proper management and treatment.
Adjusting to Life with Hives
Living with hives can be difficult and stressful, whether they are acute or chronic. The following advice will help you get used to living with hives:
-
Know what causes your hives to flare up and try to avoid those things as much as you can. Stress, particular foods, medications, and environmental factors are examples of common triggers.
-
Work with your healthcare professional to create a treatment plan that includes antihistamines, topical creams, or other medications. Follow the schedule and take your medications as directed.
-
Keep your skin moisturized and clean by following good skin care habits. Save your skin from abrasive soaps, detergents, and other irritants.
-
Keep cool because heat can make hives worse. Wear lightweight, loose-fitting clothing to stay cool, and maintain a comfortable temperature in your home.
-
Find ways to manage your stress because it can cause hives. Stress can cause hives. Think about engaging in relaxation exercises like yoga, meditation, or deep breathing.
-
It can be frustrating and isolating to live with hives; seek support. Ask your friends, family, or a support group for help. Consider talking to a therapist if you're struggling with anxiety or depression related to your condition.
-
The search for a treatment strategy that works for your particular case of hives may take some time, so have patience. Do not lose hope and exercise patience. You can control your hives and lead a full, healthy life if you receive the proper care and change your lifestyle.
Support and Resources
Individuals suffering from urticaria have access to a variety of resources. The organizations listed below provide information, support, and resources to people living with the condition:
-
The American Academy of Allergy, Asthma, and Immunology (AAAAI): A professional association of allergists and immunologists called the AAAAI offers educational materials, research updates, and a list of allergists.
-
The National Eczema Association (NEA): The NEA offers resources and information to those who suffer from eczema, hives, and other skin conditions.
-
The Asthma and Allergy Foundation of America (AAFA): The AAFA is a non-profit organization that offers information, support, and advocacy to people who have allergies and asthma.
-
The Chronic Urticaria Hives Association (CUHA): The CUHA is a non-profit group whose mission is to support, inform, and advocate on behalf of people with chronic urticaria.
-
Allergy and Asthma Network (AAN): The AAN is a non-profit group that offers information and support to people with allergies, asthma, and related conditions.
-
Skin Care Foundation: This non-profit organization aims to educate the public about skin health, skin cancer, and skin disease. They offer information about a variety of skin conditions, including urticaria.
-
GAAPP (Global Allergy and Asthma Patient Platform): The GAAPP is an international organization dedicated to improving the lives of people who suffer from allergies and asthma. They provide patients and caregivers with information and resources.
In addition to these organizations, support groups and online communities can offer valuable support and resources to people suffering from urticaria.