Welts are a form of skin rash characterized by raised, red, or white bumps or patches on the skin that are frequently itchy. Allergic reactions, infections such as viral or bacterial infections, physical stimulation, autoimmune illnesses such as lupus or rheumatoid arthritis, and stress are all causes of welts. Welts can vary in size and shape and can appear anywhere on the body. They may have a red halo around them and are typically raised, red or white. They may also be scratchable, and doing so will only make the rash worse. It can be a medical emergency when welts are severe enough to result in swelling of the face, lips, tongue, or throat. Seek medical help right away if you have severe or persistent welts, or if they are accompanied by other symptoms like breathing difficulties or facial, lip, tongue, or throat swelling.
What are Welts?
Welts are elevated, swollen markings or bumps on the skin that frequently itch or hurt. They can be brought on by a variety of things, including an allergic reaction to something that has come into contact with the skin, like food or medicine, an insect bite or sting, or an irritant, like poison ivy or specific chemicals. Welts can be pink, crimson, or even purple in color and vary in size and shape. They can develop anywhere on the body and occasionally come with additional symptoms like itchiness, discomfort, or warmth where they are located. The underlying cause of the welts will determine the course of treatment. Many welts may go away on their own within a few days, but if they are very painful or extensive, a doctor may offer over-the-counter or prescription drugs to help ease symptoms and reduce inflammation.
Medical Definition of Welts
Medically speaking, welts are described as an itchy, raised, red, or skin-colored lesion on the skin that may also cause discomfort, swelling, or warmth. Allergic responses, insect bites or stings, physical trauma, infections, and underlying medical disorders can all result in welts. Urticaria is the medical term for welts, and it is a type of skin rash characterized by the abrupt emergence of raised, irritating pimples on the skin. The duration of the symptoms determines whether the urticaria is acute or chronic. Acute urticaria typically lasts a few hours to a few days and is brought on by an allergic reaction, in contrast to chronic urticaria, which can last up to six weeks and is caused by an underlying medical condition or an autoimmune condition. Identifying and avoiding triggers, using over-the-counter or prescription antihistamines or corticosteroids, or, in severe cases, immunosuppressive medications or other doctor-prescribed therapy may be used to treat urticaria or welts.
Appearance and Sensation
The appearance and sensation of welts may differ depending on the source and intensity. Welts are typically raised, red or pink, irritating bumps on the skin. They can be circular or irregular in shape, and their sizes range from small to massive. Some welts have a pale center and a crimson rim, giving them the appearance of a "bull's eye." The sensation of welts can also vary. They are frequently itchy, but they can also be painful or tender to the touch. At the location of the welt, some people may experience burning or stinging, especially if the welt was brought on by an insect bite or sting. When an infection or underlying medical condition causes welts, they may also be accompanied by other symptoms like fever, headache, or joint pain. You should consult a physician or dermatologist for an accurate diagnosis and treatment if you have welts or any other unusual skin symptoms.
Causes of Welts
There are numerous possible causes of welts, such as:
-
Allergic reactions: An allergic reaction to food, medication, insect bite or sting, or other allergen is one of the most frequent causes of welts. The immune system produces histamine, which causes the skin's blood vessels to leak fluid and result in the recognizable red, raised bumps.
-
Physical triggers: Pressure, cold, heat, or sunlight are examples of physical factors that can cause welts to appear on the skin. The welts typically vanish an hour after the trigger is eliminated in what is known as physical urticaria.
-
Infections: Some infections, such as viral or bacterial infections, can cause welts as a symptom. Other symptoms, such as fever or headache, may accompany these.
-
Autoimmune conditions: Due to inflammation and immune system dysfunction, some autoimmune conditions, such as lupus or rheumatoid arthritis, can result in skin welts.
-
Medications: Whumps can develop as a side effect of some medicines, including antibiotics and nonsteroidal anti-inflammatory drugs (NSAIDs).
-
Stress: Histamine can occasionally be released in response to emotional stress, which results in the skin developing welts.
-
Idiopathic urticaria: Sometimes there is no known reason why welts appear. Idiopathic urticaria is what is causing this.
In order to effectively treat welts, it's critical to ascertain their primary cause. It is advised to see a doctor or dermatologist if you have welts or any other unusual skin symptoms in order to receive an accurate diagnosis and the best possible care.
Allergic Reactions
One of the most prevalent causes of welts is allergic reactions. When the body's immune system reacts inappropriately to an allergen, such as a food, drug, insect bite or sting, or other items, histamine and other chemicals are released, causing blood vessels in the skin to leak fluid. This results in the typical raised, red, itchy lumps known as welts or hives.
The severity of an allergic reaction and the individual's susceptibility to the allergen might influence the symptoms. Mild responses may result in a few isolated welts or hives, whereas more severe reactions can result in widespread welts, swelling of the face or throat, difficulty breathing, or even anaphylaxis, a life-threatening reaction that necessitates rapid medical attention. Avoiding the allergen, taking over-the-counter antihistamines or other drugs to ease symptoms, or, in severe circumstances, obtaining emergency medical care are all options for treating an allergic reaction. To minimize further reactions, it is critical to identify the origin of the allergic reaction and make efforts to avoid future exposure to the allergen. If you have symptoms of an allergic reaction, you should seek medical assistance right away.
Insect Bites and Stings
Insect stings and bites are common causes of welds. When an insect bites or stings a person, it injects venom or saliva into the skin, triggering an immunological reaction and causing a raised, red, painful welt to form. The strength of the reaction varies according to the individual's sensitivity to insect venom or saliva. Mosquitoes, bees, wasps, hornets, and ants are common insects that can produce welts from bites or stings. Insect bites and stings can cause discomfort, itching, swelling, and redness around the bite or sting site, as well as the appearance of welts or hives.
Cleaning the affected area, applying ice or a cold compress to minimize swelling, and taking over-the-counter pain medications or antihistamines to soothe symptoms are all possible treatments for insect bites or stings. An allergic reaction to an insect bite or sting may necessitate emergency medical attention in rare circumstances, especially if symptoms such as trouble breathing or swelling of the face or throat arise. It is important to wear protective clothing, use insect repellent, avoid regions where insects are widespread, and take other actions to decrease the danger of bug exposure. If you have symptoms of an insect bite or sting, seek medical assistance if they are severe or persist for an extended period of time.
Skin Irritation and Inflammation
Skin irritation and inflammation can also result in welts on the skin. This may occur as a result of a number of things, such as coming into contact with an irritant or having a skin condition. Contact dermatitis is a frequent skin irritation that can result in welts. It happens when the skin gets irritated after coming into contact with an irritant, such as chemicals, some plants, or fabrics. Contact dermatitis symptoms include red, itchy, and swollen skin, as well as welts on the afflicted area.
Eczema and psoriasis are two skin conditions that can cause welts. Psoriasis causes red, scaly patches of skin, whereas eczema is a chronic skin condition that causes dry, itchy, and inflamed skin. Sunburn, dry skin, and certain infections can also cause skin irritation and inflammation, resulting in welts. Identifying and avoiding the underlying cause of skin irritation and inflammation, applying topical corticosteroids or other medications to reduce inflammation, and taking precautions to avoid further skin irritation are all possible treatments for these conditions. In some circumstances, a dermatologist may be consulted to assist with the diagnosis and treatment of the underlying skin condition.
Types of Welts
The skin may develop a variety of welts, also referred to as hives or urticaria. The most typical types include:
-
Acute urticaria: This type of welt is recognised by the abrupt appearance of red, itchy lumps on the skin, which normally disappear within a few hours or days.
-
Urticaria chronica: This type of welt resembles acute urticaria, but the symptoms persist for six weeks or longer.
-
Physical urticaria: This type of welt can be caused by pressure, cold, heat, or physical activity. Dermatographism, which is caused by skin pressure, and cholinergic urticaria, which is caused by sweating, are two examples.
-
Urticaria from contact: This kind of welt is brought on by coming into contact with an allergen or irritant. A few examples are allergic reactions to latex, fabrics, or cosmetics.
-
Angioedema: This kind of welt is a more serious swelling that affects the subcutaneous tissue and deeper skin layers. It typically affects the face, lips, and eyes and can appear alone or in conjunction with hives.
Welts can vary in look and intensity depending on the type and underlying reason. In general, welts are raised, red, irritating pimples on the skin that can vary in size and shape. If you have welts, it is critical to determine the underlying reason and get medical assistance if the symptoms are severe or persist.
Acute Urticaria
Acute urticaria, also known as acute hives or acute urticaria, is a form of skin reaction that causes red, itchy, and raised welts on the skin to appear suddenly. Welts can form anywhere on the body, vary in size, and usually go away within a few hours or days. The most common cause of acute urticaria is an allergic reaction to a specific trigger, which can include specific foods, medications, insect bites, or allergens found in the environment, such as pollen or animal dander.
Acute urticaria symptoms include extreme itching, burning, and stinging, as well as swelling and redness of the affected area. Other symptoms, such as trouble breathing, swelling of the face, or abdominal pain, may occur in certain situations, indicating a severe allergic reaction. Identifying and avoiding the trigger, taking antihistamines or other medications to relieve itching and inflammation, and applying cool compresses or lotions to the affected area are all common treatments for acute urticaria. If the symptoms are severe or persistent, get medical help immediately because more aggressive therapies may be required to address the illness.
Chronic Urticaria
Chronic urticaria, also known as chronic hives or chronic urticaria, is a skin ailment that causes red, itchy, and raised welts to form on the skin for six weeks or longer. Welts can appear anywhere on the body, vary in size and shape, and appear and disappear over time. Chronic urticaria's underlying origin is frequently unknown, although it is thought to be related to an autoimmune reaction in which the body incorrectly targets its own tissues, causing inflammation and the release of histamine and other chemicals that produce the welts.
Chronic urticaria symptoms include extreme itching, burning, and stinging, as well as swelling and redness of the affected area. Other symptoms such as weariness, joint pain, and difficulty sleeping may occur in rare situations. Chronic urticaria treatment often consists of taking antihistamines or other medications to relieve itching and inflammation, as well as identifying and avoiding triggers that may aggravate the illness, such as certain foods, medications, or environmental allergies. More harsh therapy, such as corticosteroids or immunosuppressive medicines, may be required in some patients to manage the illness. Working together with a healthcare provider to design a personalized treatment strategy for chronic urticaria is critical.
Physical Urticaria
Physical stimuli like pressure, heat, cold, or vibration can trigger skin reactions like physical urticaria. There are several subcategories of physical urticaria, and each has its own special set of causes and signs. Several common subtypes include:
-
Cholinergic urticaria: Heat, physical exertion, or psychological stress can cause this type of physical urticaria. As a result, small, itchy pimples frequently appear on the face, arms, and chest.
-
Pressure urticaria: This type of urticaria is caused by pressure on the skin, such as that caused by belts, backpack straps, or tight clothing. It may result in large, raised welts that are itchy or painful.
-
Cold urticaria: Cold conditions, such as cold air or water, can trigger this form of urticaria. It can cause skin swelling, redness, and itching.
-
Heat urticaria: Heat exposure, such as a hot bath or sunlight, causes this type of urticaria. On the affected skin, it might cause redness, itching, and burning sensations.
-
Dermatographism: Scratching or rubbing the skin causes this sort of physical urticaria. It can cause raised, red welts on the skin in the area where the scratch or pressure was applied.
Physical urticaria is normally treated by avoiding the trigger if possible, using antihistamines or other medications to minimize itching and inflammation, and applying cool compresses or lotions to the affected skin to calm it. Immunosuppressive medicines or other advanced treatments may be required in extreme situations. If you believe you have physical urticaria, speak with a healthcare expert to establish the best course of therapy.
Symptoms and Diagnosis
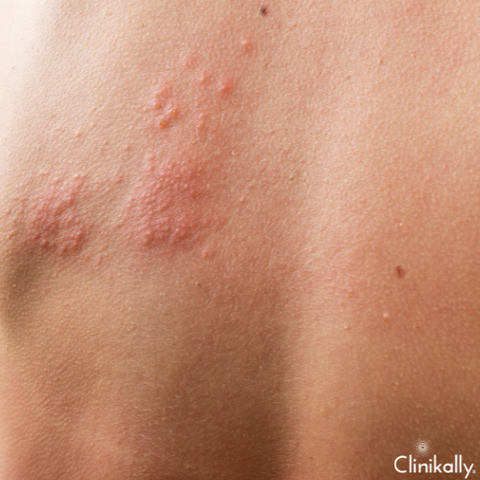
The underlying cause determines Welt's symptoms. On the other hand, welts are characterized by the development of painful or uncomfortable, raised, red, itchy bumps on the skin. Other symptoms like swelling, warmth, or a burning sensation may also accompany welts in some circumstances. To determine the source of welts, a healthcare provider will often perform a physical exam and review the individual's medical history as well as any recent exposure to potential triggers. They may also conduct allergy tests or other diagnostic investigations to help determine the underlying cause of the welts.
If an allergic reaction is suspected, the healthcare professional may recommend skin testing or blood tests to identify the allergen causing the reaction. They may also perform a physical examination to search for evidence of infection or inflammation, which could be the cause of the welts. A skin biopsy may be required in some circumstances to help detect the underlying cause of welts. A small sample of skin tissue is extracted during this process and analyzed under a microscope to find any evidence of inflammation or other abnormalities that may be contributing to the formation of welts.
Recognizing Welts
Welts are distinguished by the appearance of their skin. They often manifest as raised, red, itchy pimples of varying sizes and forms. Some welts are small and spherical in appearance, while others are larger and uneven in shape. They can also be flat or slightly elevated, with a reddish region of skin surrounding them. Welts can appear anywhere on the body and can be isolated or crowded. Other symptoms like swelling, warmth, or a burning sensation can occasionally be present along with welts. If you have welts, it is critical to be aware of any other symptoms that may accompany them and to seek medical attention if they persist or worsen over time. Your healthcare provider can assist you in determining the underlying cause of the welts and recommending appropriate treatment options to help manage your symptoms.
Diagnostic Procedures
The diagnostic approaches used to determine the underlying cause of welts vary according to the presumed cause and the severity of the symptoms. The following are some common diagnostic techniques for welts:
-
Physical examination: A healthcare provider will visually examine the affected skin area to identify welt characteristics such as size, shape, and location. They may also search for indications of infection, inflammation, or other underlying medical conditions.
-
Allergy testing: Allergy testing may be performed to identify any allergens that may be causing the welts. This may include skin prick tests or blood tests to identify specific allergens that are causing the reaction.
-
Skin biopsy: A skin biopsy may be performed in some cases to collect a small sample of skin tissue for examination under a microscope. This can aid in the identification of any underlying medical conditions or abnormalities that may be causing the welts.
-
Patch testing: Patch testing can be used to identify contact allergens that may be causing the welts. This entails applying small amounts of different allergens to the skin under a patch and monitoring the reaction.
-
Blood tests: Blood tests may be used to identify any underlying medical conditions, such as autoimmune disorders or infections, that may be causing the welts.
Once the underlying cause of the welts has been identified, appropriate treatment can be prescribed to manage the symptoms and prevent future outbreaks. If you have welts, it is critical that you seek medical attention to determine the underlying cause and receive appropriate treatment.
Treatment Options
The underlying cause and the severity of the symptoms will determine how to treat welts. Some typical welt treatment options include the ones listed below:
-
Antihistamines: These medications are frequently used to treat allergic reaction-related welts. They work by inhibiting histamine release, a chemical that causes inflammation and itching. For mild cases of welts, over-the-counter antihistamines such as loratadine or cetirizine may suffice, while stronger prescription antihistamines may be required for more severe cases.
-
Corticosteroids: Anti-inflammatory medications known as corticosteroids can help lessen swelling and inflammation linked to welts. They can be injected or taken orally as a pill. They can also be applied topically as a cream or ointment.
-
Immunomodulators: Immunomodulators are medications that aid in the regulation of the immune system and can be used to treat chronic urticaria. These medications, such as omalizumab, can help to lessen the intensity and frequency of welts.
-
Avoiding triggers: If an allergic reaction results in welts, staying away from the allergen can help stop further outbreaks. For instance, if a food allergy is to blame for the welts, avoiding the offending food may be able to stop them from appearing.
-
Creams that moisturize: Creams that moisturize can calm the skin and help with itching relief. They can also aid in avoiding dryness and irritation of the skin, which can lead to the emergence of welts.
-
Cold compresses: Cold compresses can help lessen the welts' itch and swelling. The affected area can be soothed by repeatedly applying a cold, damp cloth for a short period of time.
To determine the underlying cause of your welts and receive the best care, it's crucial that you see a doctor if you notice any of them. Most people who have welts can anticipate a full recovery because welts are frequently effectively managed with medication and other treatments.
Antihistamines
Antihistamines are drugs that prevent histamine from having its negative effects. Histamine is a chemical that the body produces when it has an allergic reaction and is what causes the itching, swelling, and redness that it results in. Antihistamines reduce the severity of allergy symptoms like welts by preventing histamine from binding to the body's receptors. Antihistamines are classified into two types: first-generation and second-generation antihistamines. Drowsiness and other side effects are common with first-generation antihistamines such as diphenhydramine (Benadryl), whereas second-generation antihistamines such as loratadine (Claritin) and cetirizine (Zyrtec) are less likely to produce drowsiness and are generally preferred for long-term usage.
Antihistamines are often used to treat allergic reactions that result in welts. They can be taken orally in the form of a tablet or liquid, or topically as a cream or ointment. Antihistamines are available over the counter, although stronger prescription antihistamines may be required in more severe situations. It is critical to take antihistamines exactly as prescribed, as taking too much or too frequently can cause drowsiness, dry mouth, and blurred vision. If you have welts, talk to your doctor about whether antihistamines are a good treatment option for you.
Corticosteroids
Corticosteroids are an anti-inflammatory medication class that can be used to treat allergic welts as well as other inflammatory skin problems. These medications operate by lowering inflammation and swelling in the affected area, which can help alleviate welt symptoms like itching and redness. Corticosteroids can be used topically as a cream or ointment, or they can be taken orally as a pill or injection. They are frequently used for more severe cases of welts or when other therapies have been ineffective. They are generally stronger than antihistamines.
However, corticosteroids can cause side effects, especially when used for an extended period of time or at high doses. Corticosteroids frequently cause side effects such as weight gain, increased appetite, mood swings, insomnia, and an increased risk of infections. The risk of osteoporosis, high blood pressure, and other serious medical conditions can also rise with the prolonged use of corticosteroids. Corticosteroids are typically used for brief periods of time and in low doses due to their potential side effects. To ensure the safe and efficient use of corticosteroids, it is crucial to work closely with a healthcare professional.
Other Medications
There are additional medicines that may be used to treat welts besides antihistamines and corticosteroids:
-
Mast cell stabilizers: These medications aid in limiting the release of chemicals such as histamine that can trigger allergic reactions. They are typically applied to stop welts from forming rather than to treat them once they have already occurred.
-
Leukotriene inhibitors: These medications prevent leukotrienes, which are chemicals that contribute to inflammation and can result in welts, from having any negative effects. They may be useful in treating welts brought on by an allergic reaction and are frequently used to treat asthma.
-
Immunomodulators: To lessen inflammation and the intensity of welts, these medications alter the immune system. They are typically applied to persistent or serious welt cases.
-
Topical anesthetics: These drugs can temporarily relieve the pain and itching associated with welts by numbing the affected area.
The medication used to treat welts will vary according to the underlying cause and severity of the welts. Working with a healthcare expert to find the best treatment approach is critical.
Home Remedies and Self-Care
In addition to medical care, there are several natural cures and self-care techniques that can help reduce the symptoms of welts. Here are some options to think about:
-
Cold compress: Using a cold compress on the afflicted area can help to lessen inflammation and itchiness. You can use a bag of ice or a cold, damp towel.
-
Bath with colloidal oatmeal: Including colloidal oatmeal in a warm bath can help calm the skin and lessen itching.
-
Aloe vera: Aloe vera gel can help lessen itchiness and redness in the affected area.
-
Calamine lotion: Using calamine lotion to soothe the skin and lessen itching can help.
-
Avoid triggers: If you know what is causing your welts, try to avoid those triggers. For example, if you are allergic to certain foods, avoid eating them.
-
Dress comfortably: Wearing comfortable, loose clothing can help ward off irritation and further inflammation.
-
Practice stress-reduction strategies: Stress can worsen inflammation and itching, so using strategies like deep breathing, meditation, or yoga may be helpful.
It's important to remember that while these treatments might help with symptom relief, they shouldn't be used in place of medical care, especially if the welts are severe or persistent. A healthcare professional should be consulted if you have welts in order to identify the underlying cause and the best course of action.
Cold Compresses
Welts and other types of skin irritation are commonly treated at home using cold compresses. Swelling, itching, and soreness can be reduced by applying a cool compress to the affected area. Cold compresses operate by restricting blood vessels in the affected area, reducing inflammation, and providing pain relief. A bag of ice or a cold, moist towel can be used to form a cold compress. Wrap the ice or towel in a thin cloth or towel to avoid direct skin contact, and apply it to the affected area for 15 to 20 minutes at a time. You can continue this step as needed throughout the day. While cold compresses can provide temporary comfort, they are not a replacement for medical care, especially in situations of severe or chronic welts. If you have welts, you should consult with a doctor to evaluate the underlying cause and determine a suitable treatment plan.
Oatmeal Baths
A calming home treatment for welts and other sorts of skin irritation is oatmeal baths. Avenanthramides, which are found in oatmeal, have anti-inflammatory qualities that can help relieve itching and discomfort. Add colloidal oatmeal to warm bathwater to produce an oatmeal bath. Colloidal oatmeal is ground oatmeal that has been finely ground and treated to make it easier to dissolve in water. Colloidal oatmeal can be found at most drugstores.
Here are the steps to making an oatmeal bath:
-
Warm water should be put in a bathtub.
-
The water should be mixed with one to two cups of colloidal oatmeal. To help the oatmeal dissolve, stir the water with your hands.
-
Spend 15 to 20 minutes soaking in the bathtub.
-
With a towel, dry your skin.
To relieve skin irritation, use oatmeal baths many times each week or as needed. While oatmeal baths can provide temporary comfort, they are not a replacement for medical therapy, especially in situations of severe or chronic welts. If you have welts, you should consult with a doctor to evaluate the underlying cause and determine a suitable treatment plan.
Avoiding Triggers
One of the most efficient strategies to treat welts if you know what is causing them is to avoid the triggers that are generating the symptoms. Here are some typical triggers and how to prevent them:
-
Allergens: If you have an allergy to certain foods, medicines, or environmental allergens (like pollen or animal dander), limiting your exposure to these things can help prevent the development of welts. You may need to consult with an allergist to identify your specific triggers and devise an avoidance strategy.
-
Irritants: Some people's skin may become irritated by specific substances, leading to welts. Soaps, detergents, and other personal care items are typical irritants. Making the switch to mild, fragrance-free products can aid in lowering your risk of getting welts.
-
Stress: For some people, stress can worsen inflammation and cause welts. Deep breathing, meditation, and yoga are all stress-reduction practices that may lessen your likelihood of getting welts when you're under pressure.
-
Heat and cold: Some people may develop welts after being exposed to extremely high or low temperatures. You can lessen your risk of getting welts by avoiding exposure to these temperatures or by dressing properly.
-
Pressure: In some people, physical pressure on the skin, such as that brought on by constricting clothing or long periods of sitting, can result in welts. Your risk of developing pressure welts can be decreased by donning loose clothing and taking frequent breaks.
It's important to keep in mind that avoiding triggers isn't always practical or possible, and some triggers can be challenging to identify. If you have welts, consult with a healthcare provider to discover the underlying reason and a suitable treatment approach.
Preventing Welts
The underlying cause will frequently determine how to prevent welts. However, the following general advice can help lower your risk of getting welts:
-
Avoid known triggers: If you have discovered particular triggers that lead to your welts, try to stay away from them as much as you can.
-
Wear protective clothing: Protective clothing, such as long sleeves and pants, is recommended if you are going to be exposed to potential allergens or irritants (such as poison ivy or insect bites).
-
Use gentle skin care products: Make sure your skin care products don't have any strong fragrances or chemicals that could irritate your skin.
-
Keep hydrated: Water is essential for maintaining healthy, hydrated skin.
-
Manage your stress: In some people, stress can exacerbate inflammation and lead to welts. Your risk of getting welts can be decreased by controlling your stress using methods like exercise, meditation, or deep breathing.
-
Get enough sleep: Sleep deprivation can weaken your immune system and increase inflammation, making you more prone to welts.
-
Maintain a healthy diet: Eating well can strengthen your immune system and lower inflammation, which can help you avoid developing welts.
A healthcare professional should be consulted if you have welts in order to identify the underlying cause and the best course of action.
Identifying and Avoiding Allergens
An essential first step in preventing welts brought on by allergic reactions is recognizing and avoiding allergens. Here are some pointers to help you recognize and stay away from allergens:
-
Keep a journal: If you have frequent welts, recording your symptoms in a journal can help you find potential allergens. Before the welts appeared, note what you consumed, drank, or came into contact with.
-
Test yourself: If you think you might be allergic, visiting an allergist for a test can help you discover the specific allergens you are sensitive to.
-
Read labels: Read the labels of food and personal care products before buying them to look for potential allergens. Look for ingredients that contain common allergens like milk, soy, shellfish, peanuts, tree nuts, and tree nuts.
-
Avoid cross-contamination: If you have a food allergy, it's crucial to keep the kitchen clean. When preparing food, use distinct cutting boards, utensils, and cookware.
-
Wear protective clothing: If you have allergies to specific plants or insects, go outside wearing long sleeves and pants.
-
Keep your home clean: Keep your home clean on a regular basis to reduce your exposure to dust mites, pet dander, and other potential allergens.
-
Use air filters: If you suffer from allergies, using air filters can help limit your exposure to airborne allergens.
It can be difficult to recognize and stay away from allergens, but doing so is crucial for avoiding welts and other allergic reactions. For advice and treatment options if you experience frequent or severe reactions, consult a healthcare professional or allergist.
Reducing Stress and Anxiety
Reducing stress and anxiety can help prevent and manage welts for some individuals. Here are some techniques that can help:
-
Practice relaxation methods: Methods like progressive muscle relaxation, yoga, meditation, and deep breathing can help you feel less stressed and anxious.
-
Exercise: Engaging in regular exercise can help lower stress and anxiety levels while also enhancing general health.
-
Get enough sleep: Aim for 7-9 hours of sleep each night as a lack of sleep can lead to higher levels of stress and anxiety.
-
Engage in social interaction: Social support can help to lower stress and anxiety. Contact your loved ones, friends, or a support group.
-
Take breaks: Throughout the day, take regular breaks to unwind, stretch, or go for a walk.
-
Seek professional assistance: If stress and anxiety are interfering with your daily life, you might want to think about getting professional assistance from a mental health professional.
Although it might not be effective for everyone, reducing stress and anxiety is an important part of overall wellness and can help some people prevent and treat welts. Determine what suits you best and give self-care and stress reduction top priority.
Proper Skin Care
In particular, welts brought on by skin irritation or inflammation can be avoided and managed with the help of proper skin care. Following are some pointers for good skin care:
-
Keep skin moisturized: Because dry skin is more susceptible to welts and other skin irritations, it is critical to keep skin moisturized. Apply a moisturizer suitable for your skin type on a regular basis, particularly after bathing.
-
Avoid harsh products: Harsh soaps, detergents, and other products can irritate the skin and cause welts. Use gentle, fragrance-free skin care products that are suitable for your skin type.
-
Wear protective clothing: If you are allergic to certain fabrics or materials, wear clothing made of cotton or silk, which is less likely to irritate you.
-
Take cool showers or baths: Hot water can dry out the skin and irritate it, so take cool showers or baths.
-
Avoid scratching: Scratching welts can make them worse and cause them to take longer to heal. If you need to stop itching, try a cold compress or over-the-counter anti-itch cream.
-
Avoid exposure to the sun: sunburn can result in welts and other skin irritations. Use a broad-spectrum sunscreen with at least SPF 30, and wear protective clothing and hats when outside.
-
Avoid triggers: If you are aware that certain items or materials cause welts, try to stay away from them as much as you can.
Proper skin care is essential for overall skin health and can assist in the prevention and management of welts produced by skin irritation or inflammation. If you experience chronic or severe welts, you should consult a healthcare expert for advice and treatment alternatives.
Complications and Related Conditions
Although they are uncommon, welt-related complications can happen. The following issues could arise:
-
Welts may be a sign of anaphylaxis, a serious allergic reaction that necessitates immediate medical attention and can occur in severe allergic reaction cases.
-
Scratching welts can cause skin breakdown and increase the risk of infection.
-
Chronic welts can cause psychological distress, such as anxiety and depression.
-
Itching and discomfort from welts can cause sleep disturbances, which can lead to fatigue and other health issues.
Other skin conditions that cause similar symptoms to welts include the following:
-
Eczema is a chronic skin condition characterized by red, itchy, and scaly skin.
-
Psoriasis is a chronic autoimmune disease that causes thick, red, and scaly patches of skin.
-
Hives are a skin condition that causes itchy, red welts.
-
Rosacea is a chronic skin condition that causes facial redness, flushing, and small, red bumps.
If you have welts or other skin conditions, you should see a doctor for a proper diagnosis and treatment. They can assist you in managing your symptoms and avoiding potential complications.
Angioedema
Angioedema is a disorder characterized by profound skin swelling, most typically around the face, lips, tongue, and throat. It is similar to urticaria or hives in appearance, but the swelling is deeper and lasts longer. An allergic reaction, drug side effects, or certain medical problems can all induce angioedema. Acute angioedema is mainly triggered by an allergic reaction to food, medication, or insect stings and lasts less than six weeks. Chronic angioedema is defined as lasting more than six weeks and is frequently related to autoimmune illnesses, hormone abnormalities, or hereditary causes. Angioedema symptoms can include:
-
Swelling of the face, lips, tongue, and throat
-
A stinging or burning sensation
-
Difficulties breathing or swallowing
-
Cramping or diarrhea in the abdomen (in cases of gastrointestinal angioedema)
The etiology and severity of angioedema dictate the course of treatment. Mild cases may not necessitate treatment, while severe cases may necessitate immediate medical intervention. Antihistamines, corticosteroids, and epinephrine are all possible treatments. Medication that regulates the immune system may be used to prevent attacks in situations of hereditary angioedema. Seek medical assistance right away if you suspect you have angioedema or are experiencing significant swelling or difficulty breathing.
Anaphylaxis
Anaphylaxis is a severe, potentially fatal allergic reaction that necessitates prompt medical intervention. It can happen within seconds to minutes of being exposed to an allergen, which could be food, medication, insect venom, or something else. Among the symptoms of anaphylaxis are:
-
Hives, itching, and redness are examples of skin reactions.
-
Face, lip, tongue, and throat swelling
-
Breathing difficulties or shortness of breath
-
Coughing or wheezing
-
Pain or tightness in the chest
-
A strong or weak pulse
-
Vomiting, nausea, or diarrhea
-
Fainting or dizziness
Anaphylaxis is a medical emergency that must be treated right away with epinephrine (adrenaline), which can help reverse the symptoms and prevent further complications. To treat the symptoms, other drugs like corticosteroids and antihistamines may also be used. After receiving emergency care, it's crucial to follow up with a healthcare provider to determine what caused the anaphylactic reaction and create a management strategy to prevent it from happening again.
When to See a Doctor
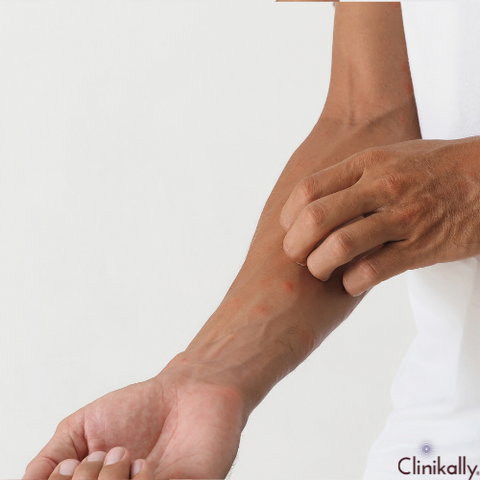
If you get welts or other skin symptoms that are persistent, severe, or accompanied by other troubling symptoms such as difficulty breathing, dizziness, or chest pain, you should visit a doctor. If you have anaphylactic symptoms such as difficulty breathing or throat swelling, get immediate medical treatment. If you have a history of allergies or know triggers for your welts, seeing an allergist or immunologist to diagnose the reason and build a care plan may be beneficial. A dermatologist may be able to help uncover underlying skin issues or design a treatment plan if your welts are chronic or recurring. You should see a doctor if your symptoms are interfering with your daily activities, causing you pain or discomfort, or if you have any other concerns about them.
Indications for Medical Attention
If you experience any of the following symptoms related to welts, you should get medical help:
-
breathing issues or shortness of breath
-
swelling of the tongue, throat, lips, or face
-
tightness or pain in the chest
-
fainting or vertigo
-
extreme itch or pain
-
large, spreading welts or a widespread rash
-
Symptoms that do not subside with self-care or at-home remedies
-
Chronic urticaria or recurrent welts
-
Symptoms that are bothersome or reduce the quality of life or daily activities
Additionally, if you have ever experienced anaphylaxis or severe allergic reactions, you should see a doctor right away because these conditions call for immediate medical attention. It is always best to seek advice from a healthcare professional if you are unsure whether your symptoms demand medical attention.
Seeking Professional Help
If you get welts or other serious symptoms, you should seek expert advice from a healthcare specialist. Make an appointment with your primary care physician, who will review your symptoms and send you to a specialist if necessary. You may be sent to an allergist or immunologist, dermatologist, or other specialist for additional examination and treatment, depending on the severity and source of your welts.
It may be beneficial to keep a journal of your symptoms before your appointment, including when they began, how long they persist, and any triggers or things that tend to make them worse or better. Bring this information, as well as any drugs or supplements you are taking, as well as a list of any known allergies or medical problems, to your consultation. Your healthcare practitioner will most likely ask you about your medical history and do a physical exam during your consultation. They may also prescribe tests to assist them figure out what's causing your welts, such as allergy testing or blood tests. Your healthcare practitioner will build a treatment plan suited to your requirements and symptoms based on your evaluation and test results. It is important to follow their recommendations and continue to communicate with them about your symptoms and any changes in your condition.
Differentiating Welts from Other Skin Conditions
Welts can be difficult to distinguish from other skin conditions due to their similar appearances and symptoms. However, the following characteristics set welts apart from other skin conditions:
-
Urticaria or hives: Welts are a type of urticaria or hives that are characterized by raised, red, or pink bumps that may itch or hurt. Hives can appear anywhere on the body and can appear suddenly, frequently within a few hours.
-
Insect bites or stings: Insect bites or stings can also cause raised, red or pink bumps that may be itchy or painful. These bumps could, however, have a central puncture mark and are frequently smaller than welts.
-
Contact dermatitis: A skin rash that develops when an allergen or irritant comes into contact with the skin is known as contact dermatitis. It is frequently characterized by redness, swelling, and itchy or painful blisters. Contact dermatitis usually appears only on the skin areas that have come into contact with the irritant or allergen.
-
Eczema: Eczema is a persistent skin condition that results in dry, itchy skin and may cause bumps or red, scaly patches. Unlike welts, which frequently result from an allergic reaction, eczema is caused by a problem with the immune system.
-
Psoriasis: A chronic autoimmune condition known as psoriasis causes skin cells to multiply quickly, resulting in thick, scaly patches or plaques that may itch or hurt. In contrast to welts, which are typically raised, pink or red lesions, psoriasis lesions can be silvery and scaly.
It's important to get a medical professional's evaluation and diagnosis if you're not sure what's causing your skin symptoms. They can assist in determining the underlying reason for your symptoms and create a treatment strategy that is specific to your requirements.
Eczema, Psoriasis, and Other Rashes
Common skin conditions like eczema, psoriasis, and other rashes can be mistaken for welts. Let's examine these circumstances in more detail:
-
Eczema is a chronic skin condition that causes skin inflammation and irritation. It is also referred to as atopic dermatitis. It can result in small, fluid-filled blisters that can rupture and crust over, as well as dry, itchy, and red skin. Although it can appear anywhere on the body, eczema frequently appears in areas where the skin wrinkles, such as in the folds of the arms or behind the knees.
-
Psoriasis is a chronic autoimmune condition that causes skin cells to rapidly accumulate, resulting in thick, scaly patches of skin. These patches are frequently red or pink in color and can be itchy, painful, or both. Psoriasis can occur anywhere on the body, but it most commonly affects the scalp, elbows, knees, and lower back.
-
Contact dermatitis is a skin rash that develops when the skin comes into contact with an irritant or allergen. It can result in red, itchy, inflamed skin that may be raised or blistered. The rash is usually limited to the area of skin that was exposed to the irritant or allergen.
-
Rosacea is a chronic skin condition that causes facial redness, flushing, and pimples. It can also cause little blood vessels on the skin's surface to become visible, as well as cause the skin to thicken and become rough. Rosacea is caused by a number of causes, including sun exposure, stress, and particular foods or beverages.
-
Pityriasis rosea is a common skin condition that primarily affects adolescents and young adults. It causes a rash of pink or red oval-shaped patches on the chest, back, and abdomen. The rash may be itchy and can last for several weeks to months.
If you have symptoms of a rash or a skin condition, it is critical that you consult with a healthcare provider for proper diagnosis and treatment. Topical or oral medications, as well as lifestyle changes to manage symptoms and reduce triggers, may be used as treatment options.
Importance of Accurate Diagnosis
Accurate diagnosis of skin disorders is critical for proper treatment and management. Different skin disorders can have similar symptoms, making differentiation difficult. A correct diagnosis can aid in determining the underlying cause of the skin issue, which could be an allergic reaction, infection, or another condition. With the correct diagnosis, healthcare providers can build an effective treatment strategy that minimizes potential negative effects. Incorrect or delayed skin issue diagnosis can cause continued discomfort, worsening symptoms, and serious complications. Some skin disorders, such as infections, necessitate immediate medical intervention to prevent the condition from spreading or worsening. In other circumstances, a misdiagnosis can result in costly and sometimes hazardous therapies or medications. If you suspect you have a skin problem or are experiencing symptoms such as welts, it is critical that you get professional medical assistance in order to acquire an accurate diagnosis and treatment plan. Dermatologists and other healthcare experts that specialize in skin diseases can make an accurate diagnosis and collaborate with you to build a treatment plan that is tailored to your specific needs.