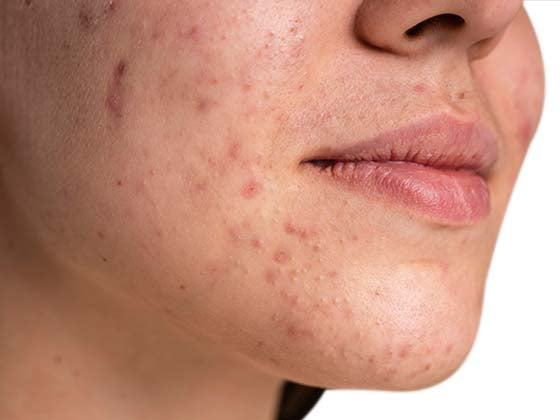
Fungal acne, also known as pityrosporum folliculitis, is a type of acne caused by an overgrowth of yeast on the skin. Unlike traditional acne, fungal acne is caused by a fungus rather than bacteria. Here is what you need to know about fungal acne:
Causes: Fungal acne is caused by an overgrowth of yeast called Malassezia on the skin. This yeast is normally found on the skin but can overgrow and cause inflammation in the hair follicles, leading to acne.
Symptoms: Fungal acne appears as small, itchy bumps that are usually uniform in size and shape. Unlike traditional acne, it is often found on the chest, back, and shoulders rather than on the face. Fungal acne may also be accompanied by redness and scaling of the skin.
Treatment: Fungal acne can be treated with antifungal medications like topical or oral antifungal creams or shampoos containing ingredients like ketoconazole, selenium sulfide, or pyrithione zinc. In some cases, oral antibiotics may be prescribed to treat bacterial infections that can occur as a result of scratching and irritating the affected area.
Prevention: To prevent fungal acne, it is important to keep your skin clean and dry. Avoid using heavy, oily products on your skin, and make sure to shower and change your clothes after exercising or sweating. Use an antifungal body wash or shampoo if you are prone to fungal acne on your body or scalp.
It is important to note that not all bumps on the skin are fungal acne. If you are unsure whether you have fungal acne or another skin condition, it is best to see a dermatologist for an accurate diagnosis and treatment plan.
What is Fungal Acne?

Fungal acne, also known as pityrosporum folliculitis, is a type of skin condition that is caused by an overgrowth of yeast on the skin. Unlike traditional acne, which is caused by bacteria, fungal acne is caused by a type of fungus called Malassezia.
Malassezia is a type of yeast that is found on the skin of most people. However, in some cases, the yeast can overgrow and cause inflammation in the hair follicles, resulting in acne-like bumps on the skin. Fungal acne typically appears on the chest, back, and shoulders, but it can also occur on the face.
The symptoms of fungal acne include small, itchy bumps that are often uniform in size and shape. These bumps can be red or white and may be accompanied by scaling or flaking of the skin. Unlike traditional acne, fungal acne is often not responsive to traditional acne treatments, such as benzoyl peroxide or salicylic acid.
Fungal acne can be treated with antifungal medications, such as topical or oral antifungal creams, shampoos, or medications. It is important to keep the affected area clean and dry and to avoid using heavy, oily products on the skin. If you suspect that you have fungal acne, it is best to see a dermatologist for an accurate diagnosis and treatment plan.
Understanding Malassezia

Malassezia is a genus of yeast that is commonly found on the skin of humans and animals. While it is a normal part of the skin's microbiome, an overgrowth of Malassezia can lead to various skin conditions, including fungal acne, seborrheic dermatitis, and dandruff.
There are several different species of Malassezia, but the most common species found on human skin are Malassezia globosa and Malassezia restricta. These species are able to break down sebum, the oil that is produced by the sebaceous glands in the skin, into fatty acids that can irritate the skin and cause inflammation.
In some cases, an overgrowth of Malassezia can be triggered by factors such as hormonal changes, stress, or use of certain medications. In other cases, the exact cause of the overgrowth is unknown.
While Malassezia can contribute to certain skin conditions, it is important to note that it is not always the sole cause. Other factors, such as genetics, environmental factors, and immune system function, can also play a role in the development of skin conditions.
To treat skin conditions associated with Malassezia overgrowth, antifungal medications, such as topical or oral antifungal creams or shampoos, may be prescribed. In addition, maintaining good skin hygiene and avoiding triggers, such as heavy or oily skin products, can help to prevent an overgrowth of Malassezia and reduce the risk of developing skin conditions.
Symptoms of Fungal Acne

The symptoms of fungal acne, also known as pityrosporum folliculitis, may vary depending on the severity of the condition. Here are some common symptoms:
-
Small, itchy bumps: Fungal acne often appears as tiny, itchy bumps that are uniform in size and shape. They can be white, red, or skin-colored and are usually clustered in groups.
-
Redness and inflammation: Fungal acne can cause redness and inflammation around the affected area, which may be accompanied by mild to moderate pain or discomfort.
-
Pimples or pustules: In some cases, fungal acne can cause pimple-like bumps or pustules, which may be filled with pus or other fluids.
-
Scaling or flaking: Fungal acne can cause the skin to become dry, scaly, or flaky, especially in the areas surrounding the affected follicles.
-
Occurs on the chest, back, and shoulders: Unlike traditional acne, which often occurs on the face, fungal acne is more likely to appear on the chest, back, and shoulders.
If you suspect that you have fungal acne, it is important to see a dermatologist for an accurate diagnosis and treatment plan. Fungal acne may be difficult to distinguish from other types of acne or skin conditions, so it is important to receive an expert evaluation to ensure that you receive the appropriate treatment.
Types of Fungal Acne

Fungal acne, also known as pityrosporum folliculitis, can present in several different forms. Here are some of the types of fungal acne:
-
Closed comedones: Closed comedones, also known as whiteheads, are small, flesh-coloured or white bumps that appear on the skin. These bumps are caused by clogged hair follicles, which can be a symptom of fungal acne.
-
Inflammatory papules and pustules: Inflammatory papules and pustules are red, inflamed bumps on the skin that can be filled with pus. These bumps can be painful and itchy, and may be a symptom of more severe fungal acne.
-
Folliculitis: Folliculitis is a condition in which hair follicles become inflamed and infected. It can be caused by a bacterial or fungal infection and can result in small, itchy bumps on the skin.
-
Seborrheic dermatitis: Seborrheic dermatitis is a type of skin condition that causes red, scaly patches on the skin. It is often accompanied by itching and flaking and can be caused by an overgrowth of Malassezia yeast, which is also responsible for fungal acne.
It is important to see a dermatologist for an accurate diagnosis if you suspect that you have fungal acne. The appropriate treatment will depend on the severity and type of the condition.
Pityrosporum Folliculitis

Pityrosporum folliculitis, also known as fungal acne, is a type of skin condition that is caused by an overgrowth of the yeast Malassezia in the hair follicles. It typically appears as small, itchy bumps on the skin, especially on the chest, back, and shoulders.
Pityrosporum folliculitis is often mistaken for traditional acne, but it is actually caused by a different type of microbe. While traditional acne is caused by the bacterium Propionibacterium acnes, fungal acne is caused by the overgrowth of Malassezia yeast.
The overgrowth of Malassezia yeast can be triggered by factors such as hormonal changes, stress, or the use of certain medications. The condition is more common in people with oily skin or those who sweat excessively.
Treatment for pityrosporum folliculitis typically involves the use of antifungal medications, such as topical or oral antifungal creams or shampoos. Maintaining good skin hygiene and avoiding triggers, such as heavy or oily skin products, can also help to prevent an overgrowth of Malassezia and reduce the risk of developing fungal acne.
If you suspect that you have pityrosporum folliculitis, it is important to see a dermatologist for an accurate diagnosis and treatment plan. They can help determine the underlying cause of the condition and recommend appropriate treatments to alleviate symptoms and prevent future outbreaks.
Causes and Triggers of Fungal Acne

Fungal acne, or pityrosporum folliculitis, is caused by an overgrowth of Malassezia yeast in the hair follicles. While Malassezia is a normal part of the skin's microbiome, overgrowth can occur due to several different factors, including:
-
Hormonal changes: Hormonal fluctuations, such as those that occur during puberty, pregnancy, or menopause, can increase oil production in the skin and create a favorable environment for Malassezia overgrowth.
-
Hot and humid weather: Hot and humid weather can increase sweating and oil production, which can lead to fungal acne.
-
Oily skin products: The use of heavy or oily skin products, such as moisturizers, sunscreen, or makeup, can trap oil and sweat in the hair follicles and contribute to Malassezia overgrowth.
-
Tight-fitting clothing: Wearing tight-fitting clothing, especially during exercise or other physical activity, can increase sweating and contribute to fungal acne.
-
Medications: Certain medications, such as antibiotics or corticosteroids, can disrupt the natural balance of the skin's microbiome and contribute to Malassezia overgrowth.
-
Weakened immune system: A weakened immune system, either due to an underlying medical condition or medication, can increase the risk of developing fungal acne.
It is important to identify and avoid triggers of fungal acne in order to prevent future outbreaks. If you suspect that you have fungal acne, it is important to see a dermatologist for an accurate diagnosis and treatment plan. They can help determine the underlying cause of the condition and recommend appropriate treatments to alleviate symptoms and prevent future outbreaks.
Yeast Overgrowth

Yeast overgrowth occurs when there is an excessive growth of yeast in the body. Yeast is a type of fungus that is normally present in small amounts on the skin and in the digestive tract. However, when the balance of the body's microbiome is disrupted, yeast can grow out of control and cause a range of symptoms.
One of the most common types of yeast overgrowth is caused by the yeast Candida albicans. This can occur due to factors such as the use of antibiotics or corticosteroids, a weakened immune system, or an imbalanced diet that is high in sugar and carbohydrates.
Symptoms of yeast overgrowth can vary depending on the location and severity of the infection. Some common symptoms may include:
-
Skin rashes or infections, such as fungal acne or ringworm
-
Digestive symptoms, such as bloating, gas, or diarrhea
-
Oral thrush, a white coating on the tongue or inside the mouth
-
Vaginal yeast infections
-
Fatigue or low energy
-
Mood changes, such as anxiety or depression
Treatment for yeast overgrowth typically involves addressing the underlying cause of the condition and taking steps to rebalance the body's microbiome. This may involve taking antifungal medications, changing the diet to reduce sugar and carbohydrates, and taking probiotics or other supplements to support gut health.
If you suspect that you have yeast overgrowth, it is important to see a healthcare provider for an accurate diagnosis and treatment plan. They can help determine the underlying cause of the condition and recommend appropriate treatments to alleviate symptoms and prevent future outbreaks.
Overactive Oil Glands

Overactive oil glands, also known as seborrhoea or seborrheic dermatitis, occur when the sebaceous glands in the skin produce too much sebum. Sebum is an oily substance that helps to lubricate and protect the skin, but excessive production can lead to a range of symptoms.
Seborrhoea can affect different parts of the body, but is most commonly seen on the scalp, face, and chest. Symptoms may include:
-
Greasy or oily skin
-
Redness or inflammation
-
Flaking or scaling of the skin
-
Itching or discomfort
-
Pimples or acne-like lesions
There are several factors that can contribute to overactive oil glands, including genetics, hormonal changes, stress, and certain medical conditions. Treatment for seborrhea may involve using medicated shampoos or topical creams to help regulate sebum production and reduce inflammation. In some cases, prescription medications such as oral antifungals or corticosteroids may be necessary.
It is important to work with a healthcare provider or dermatologist to determine the underlying cause of overactive oil glands and develop an appropriate treatment plan. In addition, making lifestyle changes such as reducing stress, avoiding harsh skin products, and maintaining a healthy diet and exercise routine may also help to improve symptoms.
Skin Microbiome Imbalance

The skin microbiome is the collection of microorganisms, including bacteria, fungi, and viruses, that live on the skin. These microorganisms play an important role in maintaining the health of the skin by helping to regulate the skin's pH, preventing the growth of harmful bacteria, and supporting the immune system.
When there is an imbalance in the skin microbiome, also known as dysbiosis, it can lead to a range of skin conditions, including fungal acne, seborrheic dermatitis, eczema, and psoriasis. The causes of microbiome imbalance can vary, but may include:
-
Overuse of antimicrobial products
-
Use of harsh skin care products or cleansers
-
Poor diet or lifestyle habits
-
Exposure to environmental toxins
-
Use of antibiotics or other medications
Symptoms of microbiome imbalance may include redness, itching, dryness, or inflammation of the skin. Treatment for dysbiosis may involve using probiotics or prebiotics to support the growth of beneficial microorganisms, reducing exposure to toxins, and making lifestyle changes such as improving diet and reducing stress.
It is important to work with a healthcare provider or dermatologist to determine the underlying cause of microbiome imbalance and develop an appropriate treatment plan. In addition, practicing good skin care habits such as using gentle cleansers, avoiding overuse of antimicrobial products, and maintaining a healthy diet and lifestyle can help to prevent dysbiosis and support a healthy skin microbiome.
Treatment of Fungal Acne

The treatment of fungal acne typically involves the use of topical or oral antifungal medications. Some common treatment options include:
-
Topical Antifungals: Over-the-counter or prescription-strength topical antifungal creams, lotions, or sprays can be applied directly to the affected areas of the skin. These medications work by killing the Malassezia fungus responsible for fungal acne. Common topical antifungal ingredients include ketoconazole, ciclopirox, and selenium sulfide.
-
Oral Antifungals: In more severe cases, oral antifungal medications may be prescribed. These medications work by killing the fungus from the inside out. Common oral antifungal medications include itraconazole and fluconazole.
-
Combination Therapy: In some cases, a combination of topical and oral antifungal medications may be necessary for effective treatment.
-
Lifestyle Changes: Making lifestyle changes such as avoiding oily or greasy products, wearing loose clothing, and maintaining good hygiene can also help to prevent and treat fungal acne.
It is important to work with a healthcare provider or dermatologist to determine the most appropriate treatment plan for fungal acne, as some treatments may be more effective than others depending on the severity of the condition. In addition, it may take several weeks or months of treatment to see significant improvement, and it is important to continue treatment as prescribed to prevent recurrence of the condition.
Antifungal Agents

Antifungal agents are medications used to treat fungal infections, including fungal acne. These medications work by either killing the fungus or preventing it from growing and spreading.
Some common types of antifungal agents used to treat fungal acne include:
Azoles: Azoles are a class of antifungal medications that work by inhibiting the synthesis of ergosterol, a key component of fungal cell membranes. Some common azole medications used to treat fungal acne include ketoconazole, clotrimazole, and miconazole.
Selenium sulfide: Selenium sulfide is an antifungal agent that works by slowing down the growth of the Malassezia fungus responsible for fungal acne. It is commonly found in medicated shampoos and body washes.
Oral antifungals: In more severe cases of fungal acne, oral antifungal medications may be prescribed. These medications include itraconazole, fluconazole, and terbinafine.
Tea tree oil: Tea tree oil is a natural antifungal agent that has been shown to be effective in treating fungal infections, including fungal acne. It can be applied topically to the affected area, but should be used with caution as it can cause skin irritation in some people.
It is important to follow the instructions of your healthcare provider or dermatologist when using antifungal agents to treat fungal acne, as some medications may have potential side effects or interactions with other medications. In addition, it is important to use these medications as directed and to continue treatment for the full prescribed course to ensure effective treatment and prevent recurrence of the infection.
Skincare Routine for Fungal Acne

Fungal acne, also known as pityrosporum folliculitis, is a type of acne caused by an overgrowth of yeast on the skin. Unlike traditional acne, fungal acne doesn't respond well to traditional acne treatments, and requires a different approach. Here is a skincare routine for fungal acne:
Use a gentle cleanser: Look for a cleanser that is free of sulfates, parabens, and other harsh ingredients that can irritate the skin. Opt for a gentle, pH-balanced cleanser that is specifically formulated for fungal acne.
Use an antifungal treatment: Antifungal ingredients such as ketoconazole, selenium sulfide, or pyrithione zinc can help to combat the overgrowth of yeast on the skin. Look for a product that contains one of these ingredients and apply it to the affected areas of the skin.
Apply a hydrating serum: Fungal acne can leave the skin feeling dry and irritated, so it's important to use a hydrating serum to restore moisture to the skin. Look for a serum that contains hyaluronic acid, glycerin, or ceramides.
Use a non-comedogenic moisturizer: Look for a lightweight, non-comedogenic moisturizer that won't clog pores. Avoid heavy creams or lotions that can exacerbate fungal acne.
Use sunscreen: Protect your skin from further damage by applying a broad-spectrum sunscreen with at least SPF 30. Look for a sunscreen that is free of oils and fragrances, and is specifically formulated for acne-prone skin.
Avoid certain ingredients: Fungal acne is often aggravated by certain ingredients, including fatty acids, esters, and polysorbates. Look for skincare products that are free of these ingredients, and avoid using oils and oil-based products on the affected areas of your skin.
Consider seeing a dermatologist: If your fungal acne doesn't improve with at-home treatments, or if you have severe or persistent acne, it's important to see a dermatologist. They can prescribe stronger antifungal medications or recommend other treatments that may be more effective.
Exfoliation

Exfoliation is the process of removing dead skin cells from the surface of the skin, typically using a physical or chemical exfoliant. Exfoliation can help to improve skin texture, unclog pores, and promote cell turnover.
Physical exfoliants are products that contain abrasive particles or tools that physically scrub away dead skin cells. Common physical exfoliants include scrubs, brushes, and sponges. It's important to use gentle pressure when using physical exfoliants, as too much pressure can damage the skin.
Chemical exfoliants, on the other hand, use acids or enzymes to dissolve dead skin cells. Common chemical exfoliants include alpha-hydroxy acids (AHAs) such as glycolic acid and lactic acid, and beta-hydroxy acids (BHAs) such as salicylic acid. Chemical exfoliants can be gentler on the skin than physical exfoliants, but it's important to choose the right type of exfoliant for your skin type and to follow the instructions carefully.
It's important to note that over-exfoliation can damage the skin, leading to dryness, irritation, and sensitivity. It's recommended to exfoliate no more than 2-3 times per week for most skin types, and to adjust the frequency and type of exfoliation based on your skin's needs. Always follow up exfoliation with a hydrating moisturizer to protect the skin's barrier.
Moisturization

Moisturization is the process of hydrating the skin to help it maintain a healthy balance of moisture. Moisturizing is an important part of any skincare routine, as it can help to improve skin texture, protect the skin barrier, and prevent dryness, flakiness, and premature aging.
Moisturizers come in a variety of forms, including creams, lotions, gels, and oils. When choosing a moisturizer, it's important to consider your skin type, as different skin types require different levels of hydration and ingredients. For example, if you have oily or acne-prone skin, you may want to choose a lightweight, oil-free moisturizer that won't clog pores. If you have dry or sensitive skin, you may want to choose a heavier, more hydrating moisturizer that contains ingredients like hyaluronic acid or ceramides.
It's important to apply moisturizer to clean, dry skin, and to use gentle, upward motions to avoid pulling or stretching the skin. You should also pay attention to the ingredients in your moisturizer, and avoid products that contain irritants or allergens that may cause irritation or breakouts.
In addition to using a moisturizer, there are other steps you can take to help keep your skin hydrated, such as drinking plenty of water, avoiding hot showers or baths, and using a humidifier in dry environments.
Topical Medication

Topical medication refers to medications that are applied directly to the skin to treat various skin conditions, such as acne, eczema, psoriasis, and fungal infections. Topical medications can come in various forms, including creams, lotions, gels, ointments, and foams.
Some common topical medications for skin conditions include:
-
Retinoids: Topical retinoids, such as tretinoin and adapalene, are commonly used to treat acne and reduce the appearance of fine lines and wrinkles.
-
Topical corticosteroids: Corticosteroid creams and ointments are commonly used to treat inflammatory skin conditions such as eczema and psoriasis.
-
Antibiotics: Topical antibiotics, such as clindamycin and erythromycin, are used to treat bacterial infections on the skin, such as acne.
-
Antifungal medications: Topical antifungal medications, such as ketoconazole and terbinafine, are used to treat fungal infections on the skin, such as ringworm and athlete's foot.
-
Calcineurin inhibitors: Topical calcineurin inhibitors, such as tacrolimus and pimecrolimus, are used to treat eczema and other inflammatory skin conditions.
It's important to follow the instructions for using topical medications carefully, and to avoid using too much or too little of the medication. In some cases, topical medications may cause side effects such as skin irritation or dryness. If you experience any side effects or have any concerns about using topical medications, be sure to speak with your healthcare provider.
Prevention of Fungal Acne

Fungal acne, also known as Malassezia folliculitis, is a skin condition caused by an overgrowth of yeast on the skin. While it can be difficult to prevent completely, there are some steps you can take to help reduce your risk of developing fungal acne:
-
Keep your skin clean and dry: Fungi thrive in warm, moist environments, so it's important to keep your skin clean and dry to help prevent their growth. Shower or bathe daily, and avoid wearing tight, restrictive clothing that can trap sweat and moisture against your skin.
-
Avoid using heavy oils and emollients: Some oils and emollients, such as coconut oil and shea butter, can promote the growth of Malassezia yeast. If you're prone to fungal acne, consider using lighter, non-comedogenic products that won't clog your pores.
-
Use antifungal treatments: If you have a history of fungal acne or are prone to the condition, you may want to use antifungal treatments as a preventative measure. Antifungal shampoos and body washes, such as those containing ketoconazole or pyrithione zinc, can be effective in preventing the growth of Malassezia yeast.
-
Be careful with makeup: Some makeup products can contain ingredients that promote the growth of Malassezia yeast, so be sure to choose products that are labelled as non-comedogenic and avoid heavy, oily products.
-
Maintain a healthy lifestyle: A healthy diet and lifestyle can help support healthy skin and reduce your risk of fungal acne. Eating a balanced diet, getting enough sleep, and managing stress can all help to promote healthy skin.
It's important to note that if you do develop fungal acne, it's a treatable condition with proper care and treatment. If you're concerned about your skin or have any questions about preventing or treating fungal acne, be sure to speak with your healthcare provider or a dermatologist.
Diet and Fungal Acne

While there isn't a direct link between diet and fungal acne, certain dietary factors can indirectly contribute to the development or exacerbation of the condition. For example, diets high in sugar and refined carbohydrates can promote the growth of yeast on the skin, which can increase the risk of fungal acne. Additionally, consuming foods that you are allergic or sensitive to can lead to inflammation in the body, which can also contribute to skin issues.
On the other hand, some foods may be beneficial for promoting healthy skin and reducing the risk of fungal acne. For example, foods that are rich in vitamins A, C, and E, as well as omega-3 fatty acids, can help support healthy skin and reduce inflammation. Examples of such foods include leafy greens, colorful fruits and vegetables, fatty fish, and nuts and seeds.
Overall, while diet may not directly cause fungal acne, it's important to maintain a healthy, balanced diet to support overall skin health and reduce the risk of skin issues. If you're concerned about your diet and its impact on your skin, consider speaking with a healthcare provider or a registered dietitian for personalized advice and recommendations.
Probiotics and Fungal Acne

Probiotics are beneficial bacteria that live in our gut and help maintain a healthy balance of microorganisms in the body. Some studies have suggested that probiotics may have a positive impact on skin health, including the prevention and treatment of fungal acne.
One theory is that probiotics can help support the immune system and reduce inflammation in the body, which can contribute to a healthier skin microbiome and reduce the risk of fungal acne. Additionally, probiotics may help to crowd out harmful bacteria and yeasts, including the type of yeast that can cause fungal acne.
There is limited research on the specific strains of probiotics that may be effective in preventing or treating fungal acne, but some studies have suggested that Lactobacillus acidophilus and Bifidobacterium bifidum may be helpful. Additionally, consuming probiotic-rich foods, such as yogurt, kefir, and sauerkraut, may also be beneficial for supporting a healthy gut and skin microbiome.
While probiotics may be helpful in preventing and treating fungal acne, it's important to note that they should be used as part of a comprehensive skincare and health regimen. If you're interested in using probiotics to support your skin health, be sure to speak with your healthcare provider for personalized recommendations and advice.
Conclusion: Managing Fungal Acne for Healthy Skin

Fungal acne, also known as Malassezia folliculitis, is a common skin condition that can be frustrating and difficult to manage. However, with proper care and treatment, it's a condition that can be controlled and minimized.
To manage fungal acne, it's important to focus on a comprehensive skincare regimen that includes proper cleansing, exfoliation, moisturization, and the use of topical medications as needed. Additionally, taking steps to prevent fungal acne, such as keeping your skin clean and dry, avoiding heavy oils and emollients, and using antifungal treatments, can also be helpful.
Other lifestyle factors, such as maintaining a healthy diet and managing stress, can also support healthy skin and reduce the risk of fungal acne. While probiotics may be beneficial for some people, it's important to speak with a healthcare provider for personalized recommendations.
Overall, managing fungal acne requires a holistic approach that addresses both the symptoms and underlying causes of the condition. If you're struggling with fungal acne, be sure to speak with a dermatologist or healthcare provider for personalized advice and treatment recommendations. With the right care and management, you can achieve healthy, clear skin.