- Types of Tinea
- Risk Factors
- Symptoms of Ringworm
- Symptoms of Athlete’s Foot
- Other Types of Tinea
- Antifungal Products To Be Applied
- Strong Anti-Fungal Medicines
- Treating Fungal Infections Naturally
- FAQs
Tinea, or ringworm, is a collection of fungal skin infections that can occur on multiple parts of the body, such as the feet (athlete's foot), scalp, groin (jock itch), and nails. Dermatophytes cause them, and they favor warm, moist environments, so they are extremely infectious. The typical symptoms are red, itchy, scaly patches, which can spread unless treated. Prevention of tinea infections requires proper hygiene, drying of the skin, loose-fitting breathable clothing, and avoidance of direct contact with an infected person or surface. Early diagnosis and treatment are important for proper control. Topical antifungal creams, powders, and systemic medications are the usual treatments for tinea infections, and mild infections can be treated with over-the-counter medications. Knowledge on prevention and treatment of fungal skin infections is important for the health of the skin and avoiding recurrence. For patients with chronic or serious infections, it is advisable to seek a healthcare provider for individualized treatment.
What Is Tinea? A Closer Look at Fungal Skin Infections
Tinea, commonly called ringworm, is a fungal infection of the skin, hair, or nails due to a dermatophyte group of fungi. They are warm- and moist-loving fungi that infect parts of the body and cause various conditions like athlete's foot, jock itch, and infections of the scalp. The infection is very contagious and can be spread through direct contact with the infected individual, dirty surfaces, or shared personal items such as towels and shoes. Tinea infections present themselves as red, scaly, itchy patches, often with a ring appearance. Although these infections are not severe, they do cause discomfort and may result in further complications if left untreated. With Clinikally, understand how proper hygiene, antifungal treatments, and lifestyle adjustments are essential in both preventing and managing tinea infections effectively.
Types of Tinea: Exploring Common Variants
Tinea, also referred to as ringworm, is a fungus infection that occurs in different regions of the body. Tinea is caused by dermatophytes, a form of fungi that finds a more favorable environment in warm and damp areas. Even though the name "ringworm" sounds threatening, it's not due to a worm but due to fungal development. Tinea infections become different according to the site of the infection, and they usually manifest themselves as itchy, red, circular rashes.
-
Tinea corporis: This type occurs on the body, producing red, ring-shaped spots that can itch. It frequently shows up on arms, legs, or torso.
-
Tinea pedis: It is commonly referred to as athlete's foot and affects the feet, particularly between the toes. It produces itching, burning, and dry, cracked skin.
-
Tinea cruris: Also known as jock itch, this type involves the groin area with red, itchy rashes that spread to the buttocks and inner thighs.
-
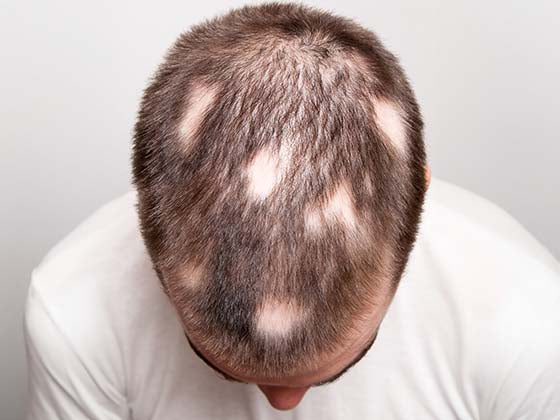
Tinea capitis: It infects the scalp, causing hair loss, itching, and scaling. More prevalent in children, this can occasionally result in secondary bacterial infections.
-
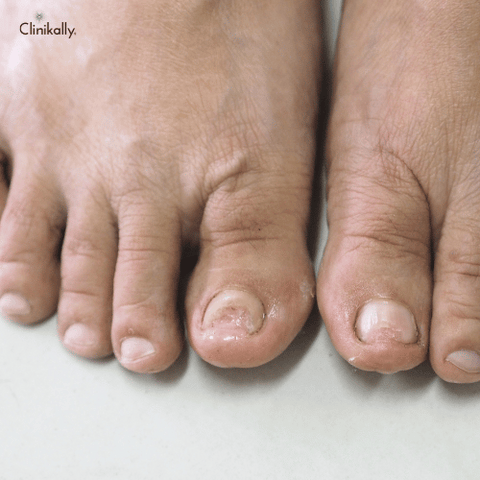
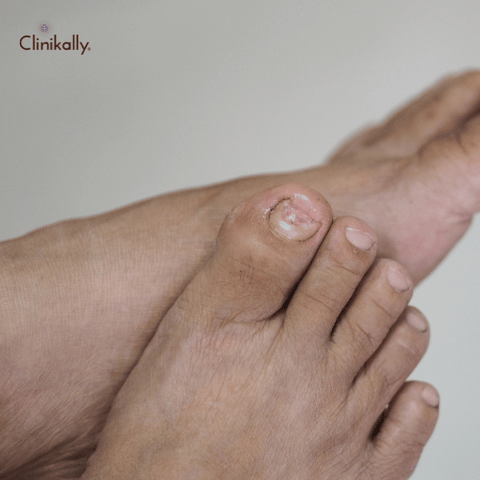
Tinea unguium: Also referred to as onychomycosis, this form is on the nails, causing discoloration, thickening, and crumbling of the nails.
-
Tinea barbae: It occurs in the beard region, causing itching, red bumps, and hair loss on the face and neck.
-
Tinea manuum: This is on the hands, resulting in scaly, itchy patches, usually developing following contact with contaminated feet or body areas.
-
Tinea versicolor: This is a fungal infection that produces small patches of discolored, lightened, or darkened skin. It often appears on the back, chest, and arms.
Though tinea infections may be irritating, they are easily treated with antifungal powders, creams, or drugs taken by mouth. It is very important to keep good hygiene, dry the infected part, and consult a doctor in case of repeated or severe infection. By identifying the various forms of tinea infections, one can learn how to avoid, control, and cure such fungal infections.
How Tinea Spreads: Understanding the Risk Factors
Tinea, which is a fungal infection brought about by dermatophytes, is very infectious and easily spreads from one individual to another. Knowing the mode of transmission of tinea and the risk factors for infection can enable you to adopt protective measures as well as guard yourself against this widespread skin disorder. Fungal spores are hardy and survive on surfaces, so it is worth knowing the routes along which tinea spreads.
-
Direct Skin-to-Skin Contact: Tinea is spread most frequently by close body contact with an infected individual. This may be achieved through casual body contact, e.g., hugging or handshaking, particularly when the fungus is on bare skin.
-
Shared Personal Effects: Tinea may be passed on using contaminated personal effects such as towels, combs, or razors. The fungus is carried by these items and can be transmitted when another person uses them.
-
Public Showers and Shower Rooms: Tinea loves warm, humid conditions and thrives in public showers, swimming pools, and shower rooms, which are ideal centers for fungal spread. Being barefoot in these places elevates the risk of catching tinea pedis (athlete's foot).
-
Contact with Infected Pets: Certain forms of tinea, e.g., tinea corporis, can be transmitted from animals, especially household pets such as dogs and cats. These pets can have dermatophytes on their coat, which can be passed to humans.
-
Dirty Surfaces: Tinea spores remain viable on surfaces such as floors, furniture, and gym equipment. Being in contact with such surfaces and then touching your skin can cause the infection to spread.
-
Weakened Immune System: People with weakened immune systems, for instance, people with diabetes or HIV, are more prone to fungal infections, including tinea. This susceptibility makes it possible for the infection to establish itself more readily.
-
Excessive Sweating: Parts of the body that sweat excessively, like the feet, groin, or armpits, are under greater risk of fungal infections. Wet conditions favor the growth of dermatophytes, making it simpler for tinea to spread.
-
Poor Hygiene and Tight Clothing: Dressed in tight, non-breathable clothing, moisture and heat get trapped, allowing tinea to grow well. Also, not washing or drying the body after sweating on a regular basis increases the risk of having a fungal infection.
Tinea infections are contagious but treatable with proper precautions. To lower the chances of spreading or getting the infection, it's essential to maintain good hygiene, not share personal items, wear porous clothes, and regularly disinfect surfaces. In case you have tinea, early treatment can help avoid complications or infect others.
Recognizing the Symptoms of Tinea: How to Identify Fungal Infections Early
Early detection of the symptoms of tinea is important to the successful treatment of the condition and avoiding the spread of the infection. Some signs of tinea infection are red, scaly, itchy patches of skin, usually with a ring-like shape, notably on the edges. The patches may become inflamed and blister in extreme cases. Based on the specific type of tinea infection, symptoms may differ: jock itch (tinea cruris) results in redness and irritation in the groin area, athlete's foot (tinea pedis) results in burning and itching between the toes, while infections of the scalp (tinea capitis) may result in scaly patches and hair loss. Tinea can further extend to the nails and cause them to thicken, become brittle, or discolor. Early diagnosis and treatment with antifungal powders, creams, or tablets are able to relieve pain and stop the infection from spreading to other areas of the body. In case the symptoms continue or intensify, it is necessary to consult a dermatologist for diagnosis and treatment.
Identifying Tinea Corporis: Ringworm on the Skin
Tinea corporis, commonly known as ringworm, is a fungal infection that affects the skin, typically forming circular, red, and itchy rashes. Despite the name "ringworm," the infection is caused by fungi, not worms. This condition can occur on any part of the body, though it is most often found on the arms, legs, and torso. Understanding how to identify tinea corporis is essential for prompt treatment and prevention of further spread.
-
Red, Round Rashes: Tinea corporis is characterized by round, red patches with raised edges. The middle of the rash might look clearer or more normal and therefore the "ring" appearance.
-
Itching Skin: Itching occurs in the infected area, which becomes worse with scratching. Itching is caused by the immune response of the body to the fungal infection.
-
Scaly and Flaky Texture: Dry, scaly, and flaky skin may appear on the rash and the surrounding area. This tends to result in peeling skin at the edges of the infection, spreading the fungus further.
-
Increasing Rash: Tinea corporis rashes tend to increase in size over time. The edges of the rash may continue to spread while the inside is clearing up, so the ring-like symptom becomes even more pronounced.
-
Bumpy or Pustular: Occasionally, the infected skin will become covered with tiny bumps or pustules filled with fluid. These look just like other skin conditions, but they are typical in more severe or untreated tinea corporis conditions.
-
Multiple Lesions: Tinea corporis can occur in multiple locations at the same time. This is possible if the infection is spread by skin-to-skin contact or from touching contaminated surfaces.
-
Mild to Moderate Pain: Along with itching, the rash may be accompanied by mild pain or a burning feeling around the rash. This pain is generally a result of inflammation brought about by the infection.
-
Location of Infection: The infection will most often be found on areas of the body that are usually exposed, like the arms, legs, and torso, but it will eventually pass to other places, including the face, neck, and hands.
Early detection of tinea corporis is the key to successful treatment. It's also essential to pursue antifungal therapy, which can either be topical or oral. Good hygiene, refraining from sharing personal items, and maintaining cleanliness and dryness on the affected area also avoid reinfection. Without proper treatment, tinea corporis may result in secondary bacterial infections or recurrent fungal infections, so early medical treatment is the solution to this common skin infection.
Tinea Pedis: The Telltale Signs of Athlete’s Foot
Tinea pedis, also referred to as athlete's foot, is a fungal infection that occurs mainly on the feet, particularly the interdigital spaces. Tinea pedis is caused by dermatophytes, fungi that thrive under warm, humid conditions. Identification of the symptoms of tinea pedis at an early stage is vital for successful treatment and for preventing spread of the infection to other areas of the body or to other individuals.
-
Itching and Burning Feeling: One of the initial symptoms of tinea pedis is a severe itching or burning feeling, especially between the toes or on the soles of the feet. This may become increasingly painful with time, especially when the feet are wet or sweaty.
-
Red, Inflamed Skin: Red, inflamed, and irritated areas on the feet can occur. The area between the toes is often more swollen or irritated, with visible redness.
-
Peeling and Cracking Skin: If the infection is allowed to progress, the skin between the toes and sole of the foot can start to peel, crack, or flake. This is because the fungus infection is destroying the outer layers of the skin.
-
Dry, Scaly Patches: Dry, scaly patches on the feet, particularly the soles, are often caused by tinea pedis. Such patches can be rough to the touch and may have an irregular texture as the skin starts shedding.
-
Blisters or Sores: Without proper treatment, tinea pedis can also cause small blisters filled with fluid to develop on the feet. The blisters can burst, resulting in sores that are painful and are prone to becoming infected with bacteria.
-
Bad Smell: The fungus infection also results in a bad smell because fungi and bacteria grow on the skin. This smell is particularly evident when shoes are taken off after being worn for extended periods.
-
Spread to Other Parts: Tinea pedis may spread to other parts of the body, particularly if you scratch your feet and then touch other parts of your skin. It can result in infections such as tinea corporis (ringworm) on the legs or tinea unguium (nail infection) if the fungus infects the nails.
-
Thickened or Colored Nails: In infection of the toenails (tinea unguium), the toenails can thicken, discolor, and even become brittle. They can start to crumble or even lift off the nail bed.
It is very contagious and can easily spread in public areas such as showers, gyms, and swimming facilities, where the fungus grows best in warm, moist conditions. Treatment is typically with topical antifungal ointments, powders, or systemic antifungal pills for more chronic infections. Daily washing of the feet and changing to dry socks frequently, in addition to not going barefoot in public spaces, can prevent athlete's foot. Early treatment is critical to control symptoms and avoid infection complications, like bacterial infections.
Other Forms of Tinea: What to Look Out For
Tinea is a fungal infection with dermatophytes that can infect various parts of the body. Although some of the most common ones include tinea pedis (athlete's foot) and tinea corporis (ringworm), there are quite a few other types of tinea that may also produce discomfort and need to be addressed. If you know how to identify the symptoms and signs of these less common types of tinea, you will be able to treat them on time and avoid worsening or spreading of the infection.
-
Tinea Cruris (Jock Itch): Tinea cruris invades the groin, thighs, and buttocks, leading to itchy, red, and inflamed skin. The rash will have distinct borders and can also spread to the neighboring areas. It occurs more in men and tends to get worse in warm, humid weather, particularly when wearing tight or non-porous clothing.
-
Tinea Capitis (Scalp Ringworm): Tinea capitis occurs mostly in the scalp and causes scaly, itchy patches that may lead to hair loss. It is found mostly in children and is very contagious. Tinea capitis most often causes small pustules, and in rare cases, kerion (swollen, painful areas on the scalp). If left untreated, tinea capitis may cause secondary bacterial infections.
-
Tinea Unguium (Nail Fungus): Otherwise referred to as onychomycosis, tinea unguium infects the nails, making them thickened, discolored (yellow or white), brittle, and crumbly. It might start off as a small spot beneath the nail and can proceed to spread, so that the nails are more difficult to treat over time. Tinea unguium might be painful, and if not treated, it could lead to permanent nail damage.
-
Tinea Barbae (Ringworm of the Beard): Tinea barbae is an infection that involves the beard and mustache regions of the face and causes redness, swelling, and pustules. It occurs more in men and may lead to hair loss in the region surrounding the infected region. This type of tinea is usually confused with folliculitis (hair follicle infection), but antifungal treatment is necessary for complete resolution.
-
Tinea Manuum (Hand Ringworm): Tinea manuum is the condition that occurs in the hands, which can result in scaly patches or itching in the skin to crack and peel. It may spread to the feet, particularly if a person with athlete's foot rubs their hands against their hands after they scratch their feet. This infection can manifest in small, rounded, elevated patches on the palm or between the fingers.
-
Tinea Versicolor (Pityriasis Versicolor): While other types of tinea result in itchy eruptions, tinea versicolor results in patches of discoloration on the skin, typically on the back, chest, and arms. The patches tend to be lighter or darker than the general skin color and are lightly scaly. The infection may become worse in warm, damp weather and is a result of an excess of yeast and not dermatophyte, so it is different from other tinea infections.
-
Tinea Faciei (Facial Ringworm): Tinea faciei appears on the face, with the exception of the scalp, resulting in red, scaly, and circular rashes. Tinea faciei is found more frequently in those with compromised immune systems and can be confused with other conditions like eczema or psoriasis. It needs to be treated with antifungal medication to prevent complications and scarring.
-
Tinea Pedis (Athlete's Foot): Although this is one of the more prevalent types, note that tinea pedis at times will spread and become a problem with the nails (tinea unguium) or the hands (tinea manuum). The fungus grows best in warm, moist areas such as locker rooms and swimming facilities and is easily transmissible from person to person.
All types of tinea are treated differently, and the most common treatments are antifungal creams, sprays, or tablets depending on the severity and site of the infection. Proper hygiene should be practiced, the infected area should be kept dry, and personal items should not be shared to avoid spreading tinea. Treatment should be done immediately to control the symptoms and prevent complications like secondary bacterial infections or permanent damage to the skin or nails.
Effective Treatment Options for Tinea: Finding the Right Solution

Proper treatment of tinea is critical to avoid the spreading of the infection and to relieve symptoms such as itching, redness, and discomfort. The appropriate treatment differs based on the location and severity of the infection. Mild infections are usually treated with topical antifungal creams, lotions, and powders, and they can easily cure cases of athlete's foot, jock itch, and ringworm. These medications usually have active ingredients such as clotrimazole, miconazole, or terbinafine that target and destroy the fungi causing infection. In severe or chronic cases, oral antifungal therapy could be ordered by a medical professional to provide deeper penetration into tissues and successful removal of the infection.
Careful adherence to treatment directions and ongoing use of antifungal products for the full course, even after the symptoms have disappeared, will help avoid recurrence. Good personal hygiene, drying affected areas, and not sharing personal items also work to prevent future infections. A healthcare professional should be consulted if the symptoms fail to improve, so the best approach is discovered for specific needs.
Topical Treatments: Antifungal Creams, Ointments & Other Products
Topical antifungal medications are the most prevalent way of treating and controlling tinea infections. Topical antifungals work well for minor to moderate fungal infections like tinea corporis (ringworm), tinea pedis (athlete's foot), and tinea cruris (jock itch). Topical antifungals are usually available as creams, ointments, powders, or sprays and can be easily purchased over the counter.
-
Clotrimazole: Clotrimazole is an antifungal medication that works by inhibiting the growth of fungi. It is often used to treat infections like ringworm, athlete's foot, and jock itch. It is usually applied to the affected area once or twice daily for up to 4 weeks. Abzorb Anti-Fungal Powder is one such topical anti-fungal dusting powder formulated to combat fungal infection as it helps absorb excess moisture, which can aggravate heat or friction rashes.
-
Miconazole: Miconazole is also a useful antifungal that acts in a similar manner to clotrimazole by inhibiting fungal cell multiplication. It may be used to treat other tinea infections such as athlete's foot and ringworm. It is usually applied twice a day for a period of up to 4 weeks.
-
Terbinafine: Terbinafine is a strong antifungal that inhibits the membrane of the fungal cell, treating fungal infections effectively. One such medication is Sebifin Cream which is used usually to treat athlete's foot, ringworm, and jock itch. Terbinafine usually works once or twice a day and can be effective in 1–2 weeks.
-
Tolnaftate: Tolnaftate is prescribed for the treatment of various fungal infections like athlete's foot, ringworm, and jock itch. It is effective in preventing the development and proliferation of fungi. The drug is applied twice a day and takes 2–4 weeks to clear the infection altogether.
-
Butenafine: Butenafine is an antifungal drug that can be used to treat a range of tinea infections, including athlete's foot and ringworm. It prevents the fungus from growing. It is usually applied once a day for 1–2 weeks to achieve a proper cure.
-
Undecylenic Acid: Undecylenic acid is a castor oil–derived antifungal and is used to treat athlete's foot, jock itch, and ringworm infections. It acts by destroying the cell membrane of the fungus. It is usually applied twice a day for optimal effect.
Topical antifungal treatments are often effective at treating tinea infections when used properly. However, if the infection persists or worsens, seeking medical advice can ensure you receive the most appropriate treatment for your condition.
Prescription Antifungals: When You Need a Stronger Approach
Whereas topical antifungal medications are sufficient for most mild to moderate tinea infection cases, prescription antifungals can be used when the infection is advanced, widespread, or resistant. Prescription antifungals usually provide more powerful formulations or other treatment methods that better target the infection. Being able to know when to get a prescription antifungal and understanding what to anticipate from them is essential in treating more chronic or severe fungal infections.
-
Oral Antifungals: In case of extensive or serious tinea infection, physicians may prescribe antifungal medicines taken orally. They attack the infection from the inside out. Topical treatments may fail, or it may be in regions that are more difficult to reach, such as the scalp or nails. Oral antifungals that are most common are drugs that block fungal cell reproduction and transmit throughout the body to attack the infection directly. Itracot-SB 130 Capsule and Kevon Tablet are such anti fungal medicines that doctors recommend. These should not be taken without a doctor's prescription.
-
Griseofulvin: Griseofulvin is among the classic oral antifungals used to treat fungal infections such as tinea capitis (scalp ringworm) or tinea unguium (fungal infection of the nail). Griseofulvin prevents fungi from dividing and growing. Griseofulvin is typically taken for weeks to months, depending on the severity and type of infection.
-
Terbinafine: Terbinafine is a strong oral antifungal commonly used for tinea infections that are resistant to topical treatments. It is commonly used in infections such as athlete's foot, ringworm, and nail fungus. Terbinafine inhibits the production of an essential building block of the fungal cell membrane, which kills the fungus. It's usually taken for a few weeks to clear the infection. Finlite Tablet is one such anti fungal medicine that doctors recommend. It should not be taken without a doctor's prescription.
-
Itraconazole: Itraconazole is an oral antifungal used to treat systemic fungal infections or infections that have spread to the nails, scalp, or internal organs. It is employed for chronic tinea infections that are not responsive to topical therapies or in more serious infection cases. Itraconazole inhibits the fungal cell membrane, and treatment times can range from weeks to months based on the infection type.
-
Fluconazole: Fluconazole is another oral antifungal medication that is usually recommended for fungal infections that are resistant to local medications. It is generally recommended for yeast infection but can also be recommended for tinea infection, especially when it occurs on the scalp or the nails. Fluconazole is generally recommended as a single dose or a short treatment regimen based on the severity of the infection.
-
Corticosteroid-Antifungal Combination: In certain instances, particularly where tinea infections result in extreme swelling, a physician can write a prescription for an antifungal drug combined with a corticosteroid to minimize swelling and inflammation. This method of treatment speeds up symptom control while still going after the fungal infection.
More Powerful Prescription antifungals, both topical and oral, act either by directly killing the fungi or preventing their proliferation. They act on various regions of the fungal cell, such as the cell wall, cell membrane, or enzymes responsible for fungal growth and development. Oral antifungals become part of the body's blood system and act across the body, but topical forms act on the affected region. More potent Antifungals provide a specific and powerful treatment for tinea infections, particularly when other topicals have not worked or when infections are more advanced. Always seek the advice of a medical professional to discover the most suitable treatment for your unique condition.
Natural Remedies for Tinea: What Works?
Although antifungal drugs are usually the best method of treating tinea infections, individuals may choose to look into natural therapies as alternative or complementary choices. Although not as powerful as prescription antifungals, some of these natural remedies have proven effective in calming symptoms and curing light cases of tinea. It is important to mention that natural treatments must be applied cautiously and, if possible, under the recommendation of a healthcare professional, particularly for more serious or long-lasting infections. Three natural remedies that can be helpful in treating mild tinea infections are mentioned below:
-
Tea Tree Oil: Tea tree oil possesses antifungal activity that will fight the fungi responsible for tinea. Mix it with a carrier oil (such as coconut oil) and apply to the infected area two times a day.
-
Apple Cider Vinegar: Apple cider vinegar contains acetic acid, which can kill fungi and help rebalance the pH of your skin. Mix with water and apply to the infected area for 10–15 minutes two times a day.
-
Coconut Oil: Coconut oil is rich in lauric acid, a compound that has antifungal properties. Use a thin application directly to the affected area 2–3 times a day to calm the skin and combat the infection.
Though natural treatments such as tea tree oil, apple cider vinegar, and coconut oil might bring relief for uncomplicated cases of tinea infection, they must be used cautiously and in combination with qualified medical advice. If your condition aggravates or does not rectify with the use of natural remedies, then a health expert should be consulted for further advice.
Preventing Tinea: Best Practices to Avoid Fungal Skin Infections
Preventing tinea infections is the best way to ensure healthy skin and prevent the itchiness that comes with fungal skin infections. The best prevention strategies start with the practice of good hygiene. Washing the skin often with mild soap such as La Moist Soap and water, particularly in high-moisture areas, will lower the risk of developing fungus. It is also very important to dry your skin because fungi grow best in moist, warm environments. Applying talcum powder or antifungal powders like Candisweat Dusting Powder in places such as the feet and groin will be able to soak up excessive moisture. Drying socks and clothes can be done. Wearing clothes and shoes that allow air to circulate, made from natural fibers like leather or cotton, prevents one from sweating excessively. Not sharing personal items such as towels, shoes, or razors helps minimize the risk of transmission. If you are a regular visitor to public places such as gyms, locker rooms, or swimming pools, wearing flip-flops and not touching surfaces directly can also help prevent fungal infections. Lastly, treating any skin injuries when they occur and preventing infection from happening can be an important factor in tinea prevention. By following these best practices, people can almost certainly minimize the possibility of getting fungal infections, ensuring overall skin well-being.